|
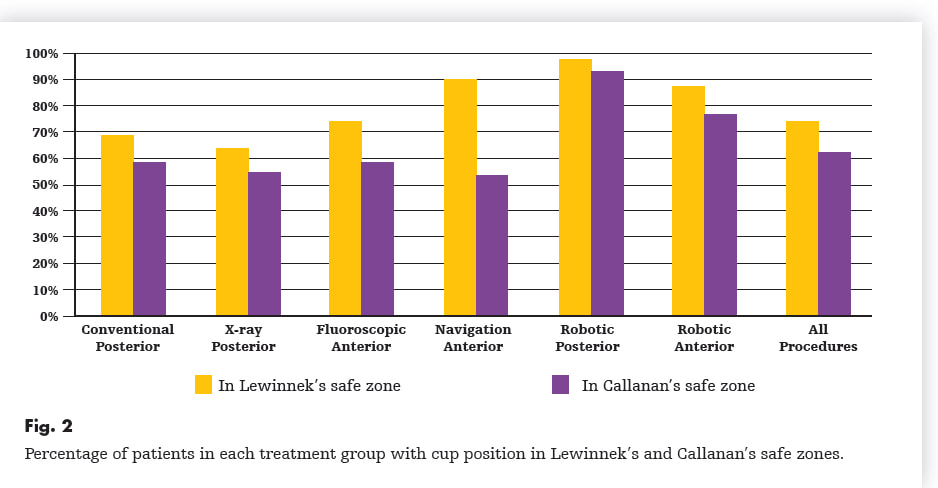
Over the years, surgeons have used a variety of surgical approaches to perform total hip replacement. Recently, there has been renewed excitement about the anterior approach. Much of this information is provided in the form of marketing/advertisement by surgeons working hard in competitive markets to grow their practice. Patients increasingly are led to believe that the anterior approach is a "different" operation. This is simply not true. The anterior approach is simply one of many approaches that can be used to perform hip replacement. I believe the data suggest the anterior approach is more about marketing than improved results. Total hip replacement is an excellent operation. It is very forgiving. When performed well, it is expected to provide dramatic improvement in pain, and quality of life for decades....regardless of approach. Why are there different approaches? Surgical approaches are anatomically safe routes between tissue planes that allow adequate exposure of deep anatomical structures. In the case of hip replacement surgery we must expose the acetabulum (hip socket) and femoral neck (top of the thigh bone). In some areas of the body there is really only one good approach. The hip, however, can be approached from the front, side, and back. Once down to bone, the operation is essentially identical, regardless of approach. Surgery, in general, has trade-offs. We need to cause controlled trauma to improve or fix something. As long as the improvement in disease outweighs the surgical trauma, the surgical procedure is worth doing. Obviously, the lower the surgical trauma the better for the patient. No surgery can be done without some trauma to the patient. In orthopedic surgery, the more accurately we can implant the joint replacement components, the better. Accuracy. With hip replacement surgery, we are replacing the patient's worn out ball and socket joint. It is crucial to place the socket (acetabular component) in a precise position. Think of the socket as a hemisphere. It is ideally aimed to be open to the side (horizontal inclination) and open to the front (anteverted). To accomplish this, the femur needs to be moved out of the way. If the cup is not ideally placed, it could allow the hip to dislocate or wear more rapidly than expected. For this reason, surgeons always look for ways to improve the position of the socket. Good surgeons are able to safely and precisely replace hips through any approach, however, most surgeons choose an approach based on their training and experience, and use it routinely. This repetition allows for greater reproducibility in outcomes. Traditionally, it was felt that the anterior approach allowed more accurate placement of the cup, with a potentially lower dislocation rate. The trade off was a higher rate of femur fracture because the anterior approach required more twisting of the femur during surgery. Recent studies (see below) bring this traditional tradeoff into question. I trained primarily with the posterior approach, and with a very low rate of dislocation using conventional (manual) alignment guides, I never felt the increased risk of intraoperative fracture warranted switching to the anterior approach. Robotic Total Hip Replacement...The most accurate total hip replacement. Now that I perform hip replacements robotically, there is absolutely no reason to consider changing approaches for accuracy. It turns out that the robotic posterior approach is the most accurate way to perform total hip replacement. But don't patients recover faster using the anterior approach? No. Most patients can bear full weight immediately and are able to go home the day after surgery with only mild pain regardless of approach. Any subtle differences, if any, patients experience between different approaches are gone within a few weeks. Risk vs. Benefit Two recent papers involving nearly 10,000 patients suggest there are potentially some significant disadvantages to the anterior approach relative to the posterior approach. The first paper found that hip replacements performed via the anterior approach became infected at over double the rate. The second paper found the posterior approach had a lower rate of complications and equal dislocation rate when compared to the anterior approach. The posterior approach appears to be the most accurate, and safest way to perform total hip replacement.
2 Comments
The future is here!
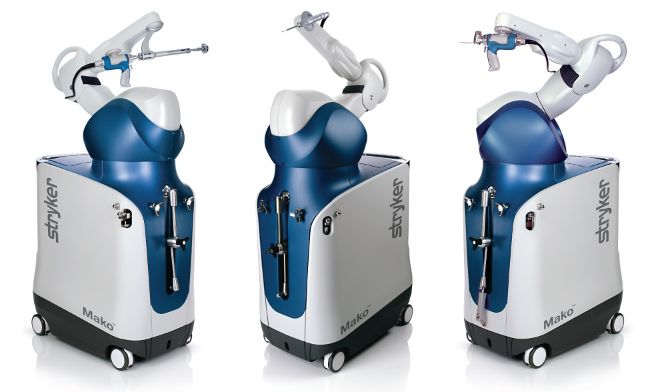
We are thrilled to announce that we are establishing a robotically assisted total joint replacement program here in Hudson, New York. We will be using the Stryker Mako system for partial knee replacements, total knee replacements, and total hip replacements. What is the big deal? Accuracy. Patients and surgeons are very fortunate in that total joint replacement is reproducible, predictable and forgiving. That does not mean it is perfect. While patients routinely report dramatic pain relief once rehabilitated, we as surgeons are thrilled when they report that their new joint feels "normal." This occurs less often than anyone would like. During surgery, we use alignment guides designed to produce certain angles, or remove a particular amount of bone. These guides have been the same for decades. Good surgeons will achieve consistent results, but even the very best surgeons will admit that there is more variability than anyone would like. This can occur for a variety of reasons, but it is impossible to completely avoid. Using a robotic arm during surgery, we can implant joint prostheses within a millimeter and a degree of the intended plan. Every time. No surgeon, anywhere, can do this using manual tools. Before you begin imagining a robotic arm like those seen in vehicle assembly, let me explain how the Styker Mako robotic arm works. Preoperatively, the patient undergoes a CT scan. The surgeon then plans the surgery virtually on the computer, determining the intended alignment and position of the prosthesis. In the operating room, the surgeon makes the surgical approach and then uses a probe to orient the robotic software to the position of the patients bones. During preparation of the bone, the robotic arm prevents anything but the exact plan from being executed. It does this passively. At no point can the robot move itself. The surgeon positions the tools and prostheses and once perfectly aligned, the robot locks the tool into this perfect position. The handpiece, which is operated by the surgeon, will not be activated until it is perfectly aligned and in a safe position. The surgeon then activates the tool, or manually impacts the prosthesis depending on the step in the procedure. The surgeon gets real-time information regarding implant position as it is happening. From the surgeon's perspective, this information is invaluable! We can adjust our plan intraoperatively if needed. We can execute our plan perfectly, every time. During knee replacement, we can balance ligaments degree by degree. During hip replacement, we can optimize acetabular (socket) placement, leg length, and offset. When dealing with complex biological systems, there will always be factors beyond our control. Robotic total joint replacement is an amazing tool, which gives us tighter control over prosthetic implantation and soft tissue balance. This will improve the function and longevity of implants for patients. Much of this website is directed toward proper rehabilitation after joint replacement. While prosthetic alignment and soft tissue balance will be improved using the Mako robot, appropriate rehabilitation will always be crucial to maximizing outcomes. |
Dr. GorczynskiOrthopedic Surgeon focused on the entire patient, not just a single joint. Categories
All
|



 RSS Feed
RSS Feed