|
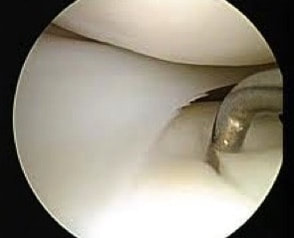
With over a million knee arthroscopic surgeries performed in the United States every year, at this point just about everyone has heard about someone having their knee "scoped." This is a quick, low risk procedure that provides relief in the majority of patients. Why then am I finding myself spending increasing amounts of time talking patients out of this procedure? It is important to understand what can be done to a knee with the arthroscope.
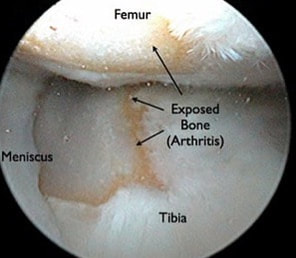
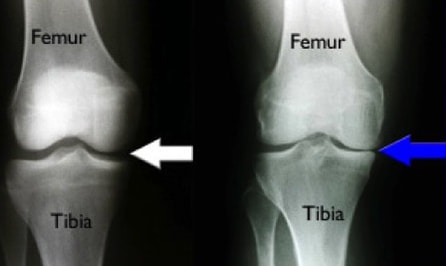
It is crucial to understand one very important thing that can NOT be done with the arthroscope. We can not "remove," "clean-up," or otherwise fix arthritis. Arthritis involves the permanent loss of articular cartilage. This is the cartilage cushion that coats the bone ends as they meet within the joint. Once articular cartilage is gone, it is gone. The solution when symptoms are unacceptable is joint replacement. Not arthroscopy. So what does all of this have to do with the meniscus? Let me describe an extremely common situation I encounter in my practice. A patient presents to my office with chief complaint of "torn meniscus." They have already had an MRI scan done. Indeed, contained within this report there is reference to a "meniscal tear." There is often reference to some degree of chondromalacia, articular cartilage degeneration, exposed bone, bone marrow edema, or subchondral cysts. All of these terms are essentially saying: "osteoarthritis." I always look at these MRI images with patients. I describe all of these pertinent findings. I explain that when there is arthritis in the same knee compartment as a meniscal tear, the pain is most likely due to the arthritis. Even if the meniscus is contributing to the pain, removing it will in no way guarantee pain relief. Many times at this point I am then asked, "so can you clean up the meniscal tear?" It is this fixation on the meniscus that I am attempting to correct. It is crucial to understand that surgically treating a degenerative meniscal tear in an arthritic knee is unpredictable at best. A patient anticipating a miraculous cure can easily be disappointed with the result. One of the most important studies we do is standing knee x-rays. Bone partially blocks x-rays whereas cartilage does not. When standing, a healthy knee has a clear separation between the femur and tibia. This separation is known as the joint space. It shows us how much articular cartilage there is. This joint space is not the meniscus, it is articular cartilage. When this joint space becomes narrowed, we know there is some arthritis. The term "bone-on-bone" arthritis refers to the complete loss of joint space on a standing knee x-ray. This is what severe arthritis looks like.
A good candidate for meniscal surgery is a patient who has been experiencing ongoing pain, swelling, and who has tenderness to palpation over the involved joint line. This is usually made worse by crouching or twisting. Standing x-rays should not reveal much, if any joint space narrowing. An MRI scan should not show articular cartilage loss or bone marrow edema. In this situation, a knee arthroscopy is a low-risk, high-reward procedure.
4 Comments
|
Dr. GorczynskiOrthopedic Surgeon focused on the entire patient, not just a single joint. Categories
All
|

 RSS Feed
RSS Feed