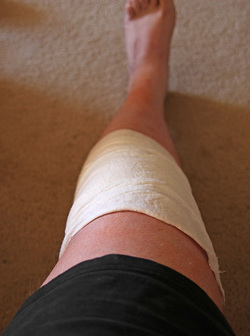
 So you finally decided to have your arthritic knee replaced. You got through the surgery just fine. As expected, you had some surgical pain, but almost immediately you realized that your arthritic pain was gone. Awesome! Things seemed to be going very nicely, and now you are home... Your knee may begin feeling tight and warm. This is normal and expected. Healing occurs in part through an inflammatory process. Inflammation shows up as swelling, warmth, and pain. You have been told to stretch, but may be questioning this recommendation now. You may be concerned that because it hurts you could be damaging yourself or your new knee. This is a very common concern. Please resist the urge to stop stretching. The knee is a complex joint. There several moving parts and potential spaces (otherwise known as tissue planes). During total knee replacement these parts are moved around , the tissue planes are opened. I think it makes sense to patients when they have some pain after surgery. But as the wound is healing on the outside, why does it feel like things are getting worse on the inside? As the healing process proceeds, the tissue planes that have been opened begin sticking together. Gradually adhesions, or scar tissue, may form between these planes preventing them from gliding properly. Initially this scar tissue is weak, but it will get stronger every day. For this reason, there is some urgency to regain range of motion as soon as possible. This is because after about 6 weeks or so from surgery this scar tissue becomes strong enough that a patient is unlikely to be able to stretch it out any more. The range of motion you have achieved at this point will be how far your knee will move permanently...without additional intervention. To better understand knee range of motion lets begin with a couple of definitions. Flexion of the knee means bending. When you sit in a chair and your feet are flat on the floor, your knee is bent, or flexed. Extension of the knee means straightened. When you stand up and your knee is straight it is extended. Now lets discuss these tissue planes a bit. 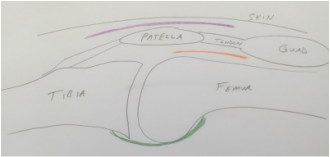 Tissue layers in the knee that must be stretched following total knee replacement. Tissue layers in the knee that must be stretched following total knee replacement. The skin must be able to slide over the kneecap (patella). The body achieves this by only loosely attaching the skin to the patella. This loose connective tissue allows motion to occur. Under abnormal conditions, fluid can collect here and create swelling. A potential space such as this is referred to as a bursa. The loose connective tissue found here is called bursal tissue. The specific space, or tissue plane, between the skin and the kneecap is called the pre-patellar bursa. It is shown in purple in my sketch. The kneecap (patella) is embedded within the tendon that attaches your thigh muscles (quadriceps) to your shin bone (tibia). A tendon is the tissue that attaches muscle to bone. The quadriceps tendon must be able to slide relative to the thigh bone (femur). The area above the patella shown in my sketch as orange is called the supra-patellar pouch. If either of these tissue planes sticks together, the knee will not be able to bend completely. In the back of the knee there is a sheet of tissue called the posterior capsule. This is green in my sketch. This tissue is irritated during surgery and will gradually tighten as it heals. If this is allowed to happen, the knee will not fully extend. So, how do you prevent a stiff total knee? It is not by walking around a lot. It is not by cycling the knee back and forth a lot. It is by gently and progressively stretching. Even though it hurts. The longer you are from surgery, the longer these stretching sessions must be because the scar tissue becomes stronger each day. Gentle progressive stretching works by taking advantage of the viscoelastic nature of biologic tissues. My basic recommendations:
google-site-verification: googlee8ce9aaf537c901b.html
400 Comments
1/8/2018 10:11:59 pm
I fx my Patella wired and screwed together 6 weeks ago. Currently passive flexion 90, active around 55-60 lots of pain. My surgeon said I should be at 90 plus by now. He said he has done all he can for now He said come back in 8 weeks. Should I get a second opinion? Can I do more. Currently CPM 6 hours a day PT once a day for 1 hour, ambulating as much as possible.
Reply
Christopher Gorczynski, MD
1/8/2018 10:48:21 pm
I would also like to see 90 degrees of flexion at the 6 week mark after open reduction internal fixation of a patella fracture. This is not always the case-for a variety of reasons.
Reply
jacqueline davey
11/26/2018 03:52:15 pm
1 yr po, 90° bend, surgeon said it's functional? 11/26/2018 05:55:22 pm
@ jacqueline davey 90 degrees is marginally functional in my opinion. I would expect you to have difficulty going up and down stairs normally, and to have difficulty standing up from a low chair using your affected knee. If it is otherwise pain-free and trustworthy, you may decide to leave it along. If, however, you do find it functionally limiting, you would be a candidate for arthroscopic lysis of adhesions with a manipulation under anesthesia. This is very likely to help you regain a truly functional range of motion if you work diligently on maintaining the range of motion your surgeon gets. It is worth discussing this with your surgeon if you are not satisfied with your level of function.
Caroline
1/19/2020 09:27:32 pm
I am 5 wks post op TRKR. My range of motion is from 68-80. My knee is tightening up so much my bend is not getting better. Would you suggest a MUA at this point or do I still have time to really push for better ROM. It is so terribly uncomfortable and extremely tight. 1/22/2020 06:01:27 pm
@Caroline... You are facing a difficult situation. If I am interpreting your question correctly, it sounds like you are stuck with a bent knee. We call that a flexion contracture. That makes walking extremely difficult.
Lissette Lopez
1/29/2020 10:52:12 pm
I had my surgery 11 weeks ago and my knee only bend 80 my surgery just bend my knee for on January 24 but while I was in surgery on November 4 they pinched my nerve so it’s traveling all the way from my leg to my back I’m in so much pain and today the spine surgery put injection on my back so I’m praying that it works because having a pinched nerve you really can’t do the things you want to do for your knee
Yvonne
2/16/2020 07:11:17 pm
I had knee surgery and I go to therapy when they bend my knee and measure it’s measure 100 and they say that not good enough and if I don’t get up up 125 I well have problems walking is that true 2/17/2020 07:42:35 pm
@Yvonne: I addressed this exact question in a recent blog entry.
Robert Mahlstedt
7/26/2020 11:11:59 am
I am 3 weeks past my total knee replacement. I worked all day yesterday in stretching and bending my knee as far as pain would allow. I iced, I walked, I exercised all day. By the end of the day I felt my knee was quite flexible. But overnight it seems like I am right back at ground zero. Is this normal? 7/26/2020 10:38:41 pm
@Robert Mahlstedt - what you describe is quite common early on after knee replacement surgery. You get it loosened up and feeling good, then you rest or sleep and it seems that you are right back where you started. This is normal, and it will be temporary. As the inflammatory process gradually winds down, I would expect you to feel less stiffness, and feel that you are making progressive gains. In the meantime, use ice to help with inflammation, and slow, long duration stretching every day. Best of luck!
Kaitlin
9/2/2020 10:52:01 pm
Hi! I’m 37. Had two scopes over the past year and a half, no medical meniscus causes me to go bone on bone coupled with localized OA on the anterior part of the knee. 9/3/2020 05:39:18 pm
@Kaitlin -
Pam Davey
9/5/2020 08:08:19 am
Thank you - the information you provided re stretching is extremely helpful. I an 66 years of age & generally fairly active. I am just over 5 weeks Post op after TKR I have an existing big scar on the inside of my femur from several osteomyelitis operations as a child then an op to remove the scar about 40 years ago & also an op to remove the infection in the scar tissue about 10 years ago I seemed to be progressing well but now have gotten very stiff & tight around my old scar closest to the knee joint I thought I was doing the right thing by cycling but now nearly overnight I can’t bend my knee enough to push the pedals around
Pam Davey
9/6/2020 01:01:16 am
Thankyou for you ideas & recommendations re stretching I am 66 years old have just had a tkr on my Right leg. I am currently 5.5 weeks post op. Seemed to be progressing well until 3 days ago when everything has stiffened seem to be limping more. As a child I had 3 operations on my inside femur for osteomyelitis 40 years ago I had the scar partially removed & 20 years ago had another op when there was an infection in the scar tissue The main pain I have now after the TKR is around the front of the old scar I can’t believe that my Physio & surgeon didn’t insist on the stretching for a considerable time
Jenn Kerr
10/24/2020 08:37:38 am
thank you sooo much for investing all the time and effort into this blog/website. I just know that the extended duration stretching is going to help me. I’m three weeks post-op, and I have almost full extension and i guess around 110 flexion - but pain and stiffness abound! 10/24/2020 04:40:09 pm
@Jenn Kerr
Jenn Kerr
10/24/2020 09:06:49 pm
Thanks again. And don’t worry, i have no intention of trying to force my hyperextension back into being.......just wondered if one being straight and the other not might make the leg lengths off kilter. :). Thanks for reassurance re S/I joint.
Michael
10/29/2020 09:39:34 pm
In the last 2 months I have had 2 knee surgeries. I had an acl reconstruction/medial meniscus repair (stitching of the meniscus). 2 months after this surgery and after intense stretching and physio, I required a MUA and arthroscopy to clear out scar tissue which was stopping my ROM in my knee. Now 2 weeks after MUA and arthroscopy and I still can’t fully extend or flex my leg. I’m stretching everyday and going to physio 3 times a week. Do you think its too early to see results or should I be seeing better results by now? I am worried that my knee will be like this forever. Would love to hear your thoughts. 11/8/2020 08:27:57 pm
@Michael
Graham
12/15/2020 05:40:05 pm
Thanks for a very informative article, will definitely do what you suggest.
Chris Kostoff
3/5/2021 07:23:47 pm
Thank you so much for doing these articles and videos. They have been very helpful. When you say 10-20 minutes per workout and 6 workouts a day stretching. For example, I can dangle my knee over the bed for 10-20 minutes at a time but knee bend that is very advanced like the placing towel under my thigh I have to do 2 sets of 5 minutes and I throw in a minute or two of more intense stretch with bend then let it hang for a minute. Do you mean 1 set during the session for 10 minutes or is it ok to do 2 sets of 5 minutes? I go by feel but have been doing what you have mentioned and it helps. I’m 4 weeks post op partial I think I’m 124 degree bend active.
Chris Kostoff
3/5/2021 07:32:01 pm
Second question since my ROM is good 4 weeks out I’m noticing 2 hours later I lose it again and stretch. I know you mentioned we have till 6 weeks to get most of ROM back. I’m only 45 athletic and prehabed like crazy before surgery so my ROM was developed. I’m trying to get as much ROM as my good leg. I’m holding on for a few more weeks on ROM so my knee loosens up. For example, I have to warm up early morning to get my shoe on with my exercise bike. I do partial rotations for 1 minute then full for 10-12 minutes then I can bend, squat, put my shoes on better. How long does it take on average to see this phenomenon go away? When do you tell your patients to cut down on stretching by a certain ROM, walking up and down steps, or post week 6-8? 3/12/2021 02:25:16 pm
The goal should be to hold the endpoint for a total of 60 minutes per day. The longer the session the better, but 5 minutes would be a good minimum. I would continue stretching until you are no longer making progress (or have achieved as much motion as you need for desired activities). Usually the knee has calmed down by 8-12 weeks postop. Younger patients often have a harder time with inflammation than older patients. This is often surprising to patients.
Charlene Collard
4/10/2021 09:39:26 pm
I had knee replacement Nov 24, 2020. The stiffness sometimes is very difficult to handle. I have pain when I try bending back to touch my butt. I watched your video and started doing the exercises you suggested. I’m having a MRI on 4/30/21 to see why I’m still having pain. Any suggestions. 4/13/2021 08:12:54 pm
@Charlene Collard. Most patients are not able to touch their heel to their butt following knee replacement surgery. If this is the only time your knee hurts, but your function is otherwise acceptable with minimal pain, I think your knee replacement is functioning normally. 6/10/2021 11:41:45 pm
Thank You I am one month post knee replacement and it’s getting stiffer every day . When I discovered your article fist thing that has made sense to me . All the PT was going no where Thank you very much I already feel better about my outcome . I will report my progress in two weeks 6/30/2021 10:52:06 pm
I love the response to this question. I had TKR 4 weeks ago and was doing the cycling motion back and forth and it made it worse. I tried the hold as long as I could flex and it works!!!
sasha
7/21/2021 11:57:36 pm
Hello.I have read all of your interesting articles on tkr. I am 4 weeks post-op. Manual pt twice a week and 3x 20 minutes of excercise daily, plus 3x 5 minutes on the hometrainer. 6x icing. Flexion is fine, beyond 120 and walking improves as I go. I use elbow crutches, mostly 1, sometimes 2. My issue is the extension. The arthrosis had me walk with a bent knee for the last 5 years and now it feels like my knee wants to snap back in that position. After pt manipulation, extension is 0 but it slowly creeps back to 5, 6 no matter how I excercise. My posture is great, compared to pre-op. I stand up straight. I just would like to be able to fully extend at all times. Thank you. 7/28/2021 08:17:39 pm
@ sasha: If you started with a flexion contracture, but are able to achieve full extension after stretching, you should be OK. It sounds like your surgeon was able to get your knee properly balanced again, and was able to regain full extension. Your soft tissues need time to adjust to this. I recommend continued stretching on a daily basis. check out the Prone Hang technique I describe in the "best extension stretch" article and also demonstrate in my videos. If you find it stiff and bent in the mornings, consider splinting it completely straight while you sleep. You can ask your surgeon for a hinged knee brace that you can lock in full extension. Keep up the good work for a few more weeks, and you should be in great shape!
Rochelle
8/27/2021 05:22:13 pm
Hello! 9/1/2021 03:49:58 am
@Rochelle - Definitely follow your surgeons range of motion recommendations, but you do not need to rely on the physical therapists to get your range of motion back. I would recommend you stretch up to the range of motion your surgeon allows on a daily basis. Expect progress for an entire year after a surgery like you underwent. Hi doc I had a distal femur fracture and patella smashed I have screws in the patella and femur I was in a cast for 7 weeks and I'm in a hinged brace now 3 weeks going on 4 and it says on the brace 20 40 60 etc but I got to roughly 60 within the first week sense then Im struggling to get to 90 on the brace and I can't understand it my physio told me I should had it there over a week ago and I'm constantly pushing it 10/5/2021 03:47:56 pm
@Jonathan - usually patients have more time following trauma surgery to regain range of motion than after knee replacement surgery. That being said- if you continue to struggle with range of motion- I would encourage you to discuss progressive static bracing, with something like Joint Active Systems (JAS), with your surgeon.
I have a question. I had a RTKR on 12/8/21. I am around 0 straight and 85 bending. I'm 4 weeks post op. 1/22/2022 01:45:52 pm
@Amy
Frank
2/16/2022 07:20:30 pm
I am 1 week post op and I have about 20° bend in my knee. It feels extremely stiff, painful and I have zero feeling in my quads. I can't do any of the physio exercises that involve engaging my quads to lift my leg off of the ground. Is this concerning? I'm worried the surgery hasn't worked
Sandy Pyle
2/24/2022 09:54:45 pm
What causes my knee to go absolutely tight so I can’t move it 2/26/2022 02:45:43 pm
@Sandy Pyle - Assuming your knee replacement was reasonably balanced at the time of surgery (and the vast majority are) there is nothing that would explain complete inability to move your knee other than poor pain control/tolerance or inadequate rehabilitation effort. Many people have a hard time relaxing into the stretch. Unfortunately, this is a necessary requirement to rehabilitate properly. 2/26/2022 03:03:53 pm
@Frank - I would encourage you to dedicate yourself to a daily stretching regimen as I describe throughout this website. Check out my videos for a demonstration. This is not a matter of your surgery "working" or not. It is crucial to get your knee moving at this point, as it will tend to get stiff if you delay this effort. Ideally you will be at a minimum of 0-90 degrees by 2 weeks from surgery, and at a minimum of 0-120 by 6 weeks from surgery.
anita
6/1/2022 01:17:37 pm
Thank you so much for this. I am two weeks post TKR and had been doing the short duration stretches that, as you point out, most practitioners suggest--with not much progress.
Marie
6/12/2022 01:44:37 pm
I wish I had read your article before. I had surgery on 3/16/22 in a Surgery Center with a nerve block and a cocktail of drugs before the block. I was released the same day and was so nauseous that I had to leave PT the very next day. The nausea continued and my knee was so stiff and I fell behind with exercising. As a result, IA was scheduled for a manipulation at five weeks post surgery. The manipulation did not improve my bend and I was still stiff afterwards. I’ve changed physical therapist and they were more accommodating and hopeful for me. I am now 12 weeks post op and I am at 100°. So my question to you is, after reading your article, I will continue with stretches rather than go on the bike and hoping that I can still gain more flexion even though I am way behind. You state that most people after six weeks are going to stay with that particular band, in my case I hope not. Have you seen other cases like myself that can continue to improve?
Barbara smith
6/17/2022 01:24:35 pm
THIS is what I needed to hear!! Sustained pressure to get Flexion ….. thank you thank you… great info 🤗 7/9/2022 02:25:53 pm
@Marie - If you diligently stretch on a daily basis, for long durations, it is possible to make gains beyond the first 6 weeks. You will need to work harder than most since you've already required a manipulation. 9/17/2022 07:23:55 pm
Hi 9/24/2022 05:07:16 pm
@Christina McRae - Irritation from the wires/hardware used to repair a patella fracture is very common. This is so commonly the case, I usually discuss the eventual need to remove this hardware with the patient before we ever do the initial fracture repair surgery. I would expect improvement for a year or more following your most recent surgery. It takes a long time for soft tissues to calm down following trauma/surgery. I would recommend continuing to stretch and massage the knee on a daily basis. Expect slow but steady recovery for months.
Trey Wilson
1/5/2021 04:28:40 pm
I am 7 1/2 weeks post op for a fractured patella. I had 1 screw and a figure 8 done during ORIF surgery. The scar has healed nicely and I have complete extension. However, my surgeon did not recommend moving the knee until about a week and a half ago, in which time I have went from about 40° flexion to 67° flexion. I visited my ortho today and he is recommending manipulation under anesthesia but I don’t want to have it done due to anesthesia concerns and scared of complications. Do you believe that your method of extended flexion could help me get to at least 90° or further without manipulation under anesthesia? I am not currently insured and money is also a concern for the MUA. I have 6 days to inform the surgeon if I want to have to procedure done or not. Thank you for your time.
Reply
Anne
2/11/2021 12:17:33 pm
I'm five years post full knee replacement. When I try to do a seated figure-four stretch, I can feel the replaced knee pull. Is there any risk to doing this kind of stretch with a knee replacement?
Reply
2/14/2021 10:22:08 am
While it is not unsafe to put a total knee replacement into the figure-four position. I would not recommend forcing it into this position or trying to stretch in this way. You are essentially trying to bend the knee sideways- which is not normal, and not helpful for function. All it will do is stretch out your lateral collateral ligament, possibly leading to symptomatic instability in the knee that could require revision surgery to correct.
Jose
4/13/2021 01:21:18 am
I am two months removed from TKR and I feel I’m not where I should be. I go to therapy three times a week and constantly working on the flex at home with lunges using the stairs. According to therapist I’m at 90° easily and to 100° when I push it. But that’s when I’m sitting down and feet NOT touching the floor.
Reply
4/13/2021 08:04:34 pm
I would recommend a manipulation under anesthesia. This is a quick, simple, routine procedure. You do not need to fear this, it is very likely to help you. A 90-100 degree arc of motion at this point is not optimal for good long-term function. Waiting much longer will require arthroscopic lysis of adhesions, which entails significantly more risk than a simple manipulation.
Jose
6/23/2021 11:27:07 pm
Good evening doc 6/28/2021 12:50:10 pm
Thank you for the update. It sounds like your hard work is paying off. Nicely done!
Lajuna fife
4/18/2021 03:30:17 pm
Thank you so much for the exercises I enjoyed my surgery is 3 years older still gets deftness but thank you for give me some tips on how to make it better God-bless
Reply
Lajuna Fife
4/18/2021 03:32:18 pm
OK thank you so much I love the exercises I would do that that will help I need to get better I'm a senior citizen I will be 72 years old thank you so much God-bless
Reply
Robert Lulek
9/1/2021 12:48:16 am
I was told to be very careful how low I bend my knee that I can damage the joint and I could loosen the cement if I’ve been to low is this true? I know I can go asked to grass but the doctor told me that I can damage the unit is it possible or is the doctor just being cautious?
Reply
9/1/2021 03:11:49 am
Cement is very strong in compression. Simply bending your knee will not cause cement to loosen. Applying significant shock to your knee in a deeply flexed position (for example by falling onto a flexed knee) could apply a shearing load to the tibial component (particularly if it is a posterior stabilized design) which could damage the fixation. Simply bending your knee deeply is safe.
Margaret Bartlett
9/5/2018 06:04:51 am
Thank you so much for this advice. I am 3 weeks post op tkr and nearly bought a small pedal machine last night and also went for a longish walk. Woke up this morning feeling very stiff then found your article. Also holding the knee bend for minutes rather than seconds has given me a breakthrough in my recovery.
Reply
11/5/2018 08:43:16 pm
Glad to hear that extended stretching is helping you. Consistency (no days off) and long duration, progressive stretching definitely seems to be the most effective, and least irritating method to rehabilitate total knee replacements.
Reply
Barb Smith
6/17/2022 01:54:35 pm
I am 74, 5 wks out…and this is the richest information from a professional I could have hoped for. Bend and HOLD‼️
Barb Smith
6/17/2022 01:51:54 pm
This is the very reason I am now Optimistic and the one simple question I had was answered… bless this dr for seeming to know me 💕
Reply
C M Allan
11/5/2018 06:45:08 pm
Thank you for this really helpful information. I'm finding the more lengthy stretches are making all the difference and I've stopped being quite so scared of splitting the scar when pushing further with the knee bends. The exercise involving hanging my knees over the side arm of the sofa is really helping get rid of the deep ache from where the tourniquet was positioned during surgery. Why is that?
Reply
11/5/2018 08:44:08 pm
I am pleased to hear that extended the duration of stretching is helping you to make progress with your total knee rehabilitation. Stretching over the arm of the sofa allows your muscles to relax during the stretch. Because the tourniquet creates mild trauma to your thigh muscles, allowing them to relax while they are being stretched is probably why you find this helpful. All too often I hear about physical therapy sessions that sound like torture sessions, or strength contests. Gentle, progressive, long duration stretching makes this process much less unpleasant. Thank you for the comment, and keep up the good work!
Reply
Barb Smith
6/17/2022 01:58:32 pm
Thank you for your saying professionally what I believe allows us to get rom without screaming in pain. A lot of whimpering tho🙃
Bob McWilliams
11/16/2018 02:08:09 am
Dr. Gorczynski,
Reply
11/26/2018 05:36:51 pm
This does sound like some scar tissue. To gain more range of motion at this point, you really need to focus on prolonged stretching exercises, maintaining stretches for 30 minutes or longer, multiple times per day if possible, and every day. Since scar tissue tends to contract over time, it is normal to feel the need to work at range of motions exercises sometimes for many months.
Reply
Bob McWilliams
11/27/2018 08:30:17 am
Thank you for your reply. I’m clear on your advice for stretching a minimum of 1 hr several times a day if possible.
Bob McWilliams
11/16/2018 02:18:56 am
Dr. Gorczynski, I’m sorry but I did want to add, when I exercise ( bike, stretching etc ) the band tightens a lot right afterwards. After a good nights rest it relaxes to its normal tightness which is tight enough it’s very aggravating and in a way dehabilitating.. Thank you
Reply
11/27/2018 09:05:28 pm
It is definitely ok to continue riding the recumbent bike as well as progressive strengthening exercises. A simple manipulation is unlikely to be very effective beyond 6-8 weeks maximum. I recommend that you continue doing exactly what you have been doing. Particularly working for long periods on regaining deep flexion. I have seen patients gradually improve their range of motion for up to an entire year from surgery. Persistence and patience will usually pay off. Ice and anti-inflammatory meds will assist you. If, at a year from surgery, you have not regained a range of motion that is acceptable to you, you could consider undergoing arthroscopic lysis of adhesions and manipulation. But, this is not something I would encourage you to do at this point because there is an excellent chance you will correct this on your own.
Reply
Jenn Kerr
11/4/2020 11:20:12 am
Hi Dr. Gorczynski, 11/8/2020 07:57:25 pm
@ Jenn Kerr: At only 4.5 weeks, with 125 degrees of motion I think you are doing just fine. I would continue stretching and icing as you describe. Maybe ease back on the biking a bit and focus more on slow, gentle stretching to maximize your range of motion over the next few weeks. You will improve for many months yet to come. While it is easy to get frustrated, patience and persistence are the key to an optimal result.
Cathleen
1/3/2019 05:18:07 pm
I am 6 weeks post knee replacement. I achieved 115 deg. range of motion at 10 days post op. I now have 121 deg. ROM but don't seem to be progressing beyond that. I have been relatively pain free but my knee is very stiff. I am very flexible and do extensive stretching 5 times a week. I will begin stretching daily per your advice. I will begin holding my stretches longer.
Reply
1/4/2019 11:51:02 am
A 121 degree arc of motion is excellent, and should be sufficient for all reasonable activities following total knee replacement. It is possible to regain even more motion, but this takes a great deal of work and is not a guarantee of better function. Scar tissue tends to thicken and contract over time. This could be why you are feeling a bit stiffer. Thankfully, this process does not last forever. I would expect this feeling of increasing stiffness to end over the next couple of months. Simply continue gentle, long duration stretching to maintain (or slightly improve) your already excellent range of motion. As for the 1.5 pound weights, if they are causing irritation, I would discontinue them. Simply walking, riding your resistance bike with low resistance, and time will help you to regain function. Gradually add double leg squats, then consider single leg squats, holding something to help with balance.
Reply
Cathleen
1/3/2019 05:20:07 pm
Sorry I forgot to mention on my previous post that I am a 68 year old woman in excellent health.
Reply
Cathleen
1/4/2019 01:55:09 pm
Dr., thank you very much for your encouraging reply. You have saved me worry and second guessing my progress. Very much appreciated!.
Reply
1/4/2019 02:29:08 pm
I do have patients that either don't want or don't tolerate narcotic medications and are similarly able to rehabilitate their total knee replacement using only ice, tylenol, and NSAIDS. The regional anesthetic block we use definitely makes a big difference for the first 20+ hours or so. Best of luck on your second knee replacement! The nice thing is that after this....you have no more knees to work on....
Reply
Sharon
1/13/2019 11:37:24 pm
Dr., I'm only 5 days post op from my TKR surgery and have yet to have my follow-up appt. with my surgeon or my first PT session. I'd been improving daily... less pain and discomfort... easier to walk and stretch. I've been doing my exercises religiously and then suddenly today my swelling and stiffness increased. It actually feels like I have an invisible ace bandage stretched around my knee! I've continued with my stretching exercises and am actually even holding a stretch longer... but this stiffness continues. Is this temporary or should I be concerned about some longer lasting effect? Thank you so much for your reply.
Reply
1/14/2019 09:46:28 pm
Your experience is not unique. It is common for patients to feel that recovery is quite easy for the first few days following surgery and then feel that their progress becomes much more difficult. This is so common, in fact, that we tell our patients to expect the second week to be less pleasant than the first.
Reply
1/17/2019 04:59:12 pm
I am 10 weeks post-op TKA. My flexion has varied of late from 125 to 127 with passive assistance. I have maintained a slight degree of swelling which my PT assures me is not impeding my progress. However, my walking has been consistently sub-par and in the last few days I've developed the that band that so many people have referened. I was very interested in your information about stretching, which my PT hasn't instructed me to do. Since reading your blog, I've been doing prolonged stretching for a couple of days and plan to continue. At times it seems to be helping, but I wonder if I've gotten to this information too late in my recovery and will need more aggressive treatment by my surgeon.
Reply
1/17/2019 08:39:12 pm
If you have achieved 127 degrees of flexion and have full extension, you should be in great shape. I would expect an excellent result. At this point I would recommend simply maintaining the range of motion you have achieved, and allow the inflammation to subside gradually as your knee heals. Patience is key. There is no reason for you to be anxious at this point, the hard work is behind you. At this point I would expect your knee to gradually settle down and feel better and better as months go by.
Reply
Melissa C
5/11/2019 08:15:47 am
I cannot even imagine 127 degrees! Wow!! I am 10 days post op and have struggled to get to 70 degrees. I simply cannot believe how extremely tight the knee is, already. I have read through all of the emails and will continue to work at holding the flex position for a longer period of time. Thanks for all of the information!! 5/12/2019 11:02:30 am
@Melissa C
Phyl
1/23/2019 01:29:33 am
I am a 70 year old female 7 weeks out from TKR. I had my right knee replaced in 2017 and now my left knee Dec 2018. I have that tight band that has been spoken about on here and only 90 flexion so far, it was stuck at 78 for 3 weeks. I’ve just started doing the longer stretches you recommended and already I can feel the difference. I think my Physio will be pleasantly surprised at my progress so far. I was too frightened to “push it” as I thought I would break something. Thank you for your suggestions they do help!
Reply
1/25/2019 10:49:30 am
It definitely sounds like you got off to a bit of a slow start. 90 degrees always seems to be a "sticky spot" with regard to range of motion.
Reply
Cheryl
1/23/2019 11:29:05 am
I had my first total knee replacement on 11/14/18 and the second one in 12/26/18. The first one was a breeze - the second one, not so much. Four weeks post surgery, I am having trouble even reaching 110 range of motion. My incision is healed yet, the sensitivity is nearly unbearable. I can’t tolerate even a light cloth touching it. I do the stretching exercises as recommended and still have therapy twice weekly. At the last visit, the therapist found an area that was extremely sore, to the right and back of my knee. He suggested I have damage to a tendon and recommended self massage. Could this be a barrier to healing?
Reply
1/25/2019 10:41:41 am
Every patient has a somewhat different experience when rehabilitating a joint replacement. A subsequent joint replacement can even feel different to the same patient. In my opinion, 110 degrees at 4 weeks is fine. I would recommend continuing to stretch for long periods of time as I recommend elsewhere in this website. The longer the better. I would expect another degree or 2 of improved range of motion for another couple of weeks time. That should allow you to regain at least 120 degrees of motion. This should be more than adequate for all desired activities.
Reply
Kevin
1/23/2019 08:17:06 pm
Dr. Gorczynski:
Reply
1/25/2019 10:35:38 am
It is very easy to become a bit impatient when rehabilitating after total joint replacement. It is important to understand that the healing process truly takes at least a year(and perhaps even longer) to be complete.
Reply
Karen
2/9/2019 02:37:55 pm
Hey Doc,
Reply
2/9/2019 08:03:19 pm
The purple in the diagram above represents the tissue plane between the skin/fat in the front of the knee and the kneecap (patella). These tissues must slide relative to each other to allow normal knee flexion. That being said, your 125 degrees of flexion suggests well done rehabilitation, and I doubt your range of motion is interfering with stairs.
Reply
Melisa Brubaker
2/9/2019 03:10:27 pm
I am 61 yrs young, I had both Osteo knees replaced using Conformis, 6 months ago 8/9/18..Before hand I started exersizing, riding a bike, & swimming to get in better shape before surgery..I had excellent exstension after surgery, everything went well, but my right knee more often that not is super tight at times, feels like a tight band around the knee, and up into my inner area & front of leg..like a pulling..I have continued with exer. 3 x a wk for 30 minutes, & I walk 15 to 30 min. every day on my treadmill as well as 15 min 3x a wk on my bike..Also my scar is darker on this knee..My left knee feels great other than a little stiffness if I sit too long..Can u suggest anything I might try? I also eat healthy to try and improve..I rarely do steps there are none in my home..could that be it? tks so very much!
Reply
2/9/2019 07:56:38 pm
From your comment, I presume both knees were done under the same anesthetic. Thus, both scars should have similar appearance. While I would expect continual improvement for up to an entire year or more from surgery, it is strange that your knees feel so different. If this is significantly irritating to you, it is worth discussing this with your surgeon to see if he/she recalls any differences intra-operatively, or if there is any soft tissue balance or range of motion difference between your knees. If your range of motion is not symmetric, I would focus on long duration stretching in an attempt to equalize and maximize your motion bilaterally.
Reply
Melisa
2/11/2019 12:35:11 pm
Thank-you!
Miriam
2/9/2019 09:26:03 pm
My knee is so stiff and 8 weeks after surgery what can I do to help this. I stretch every day with no relief.
Reply
2/9/2019 10:03:14 pm
If you are not happy with your range of motion at 8 weeks postoperatively, you could be a candidate for manipulation under anesthesia. I consider this a way to "catch-up" to where you should be at this point. It is important not to delay. I usually perform this when needed at 6 weeks post-op. Much beyond this, the scar tissue has become too robust to make much gain...in this situation an arthroscopic procedure needs to be performed first to cut the scar tissue prior to manipulation. Obviously, an invasive procedure is much less desirable than a simple manipulation. Therefore....call your surgeon this week to discuss manipulation ASAP.
Reply
I had right knee replaced jan 15 2018. I have had pain on left side of that knee since. Had arthroscopic sept 7 to break up scar tissue and bend. I was able to bend to 121 after that surgery but with great pain. My pain is worse and range of motion is too. I still go to gym twice a week. It usually takes me a few days to get over my work out which is not that strenuous. I did not have much pain prior to surgery unless I had to walk great distances (shopping, yard work). I have had a nerve block and nerve ablation (very painful). So far no relief. What do I do now? Live in pain with a stiff knee? Not what I planned when I retired. I am 69 and in great physical shape except for the knee. My mental state is suffering too.
Reply
2/10/2019 11:47:54 am
A stiff knee can be very frustrating- both to patients and to surgeons. Assuming the knee was properly balanced during surgery, a stiff knee suggests inadequate rehabilitation (stretching) in the early postoperative period. Once stiff, regaining normal motion without pain is very difficult. That is why I suggest the key is to regain full functional range of motion within the first 6 weeks postoperatively.
Reply
2/10/2019 11:55:25 am
The reason I focus so much on long duration stretching is that your tissues are viscoelastic. That means they will yield to long duration tension.
Reply
Miriam Lunk
2/14/2019 08:07:34 pm
I am 8 weeks out of total knee replacement. Rangeof motion is 127 . But I am in more pain and tne knee feels stiffer. I stretch every day. What can help this.
Reply
2/27/2019 09:53:22 pm
Time, ice, anti-inflammatory medication, continued stretching, and patience.
Reply
Nancy B
2/19/2019 12:01:54 am
I am 12 weeks post op after a patella fracture. I was in an immobilizer for the first 4 weeks. My rom was only 60 degrees at 5 weeks of PT so I had an MUA. It is now 2 weeks after the MUA and I am at 90 degrees. Do you think it is possible with your suggestions for stretching along with intensive PT to keep improving the rom or is it too late to have much of a change now? I really want to know the truth but no one seems to know the answer.
Reply
2/27/2019 09:57:07 pm
After an injury like you had, treated as yours was, I think you should expect progress with regard to range of motion for many months to come. Slow, steady, prolonged stretches are the best way to improve your range of motion. It is important do stretch as often as possible, for as long as possible, every day. Check out my article on use of a yoga strap to help.
Reply
Nancy B
3/3/2019 11:59:21 pm
Thank you for your reply and for a wonderful, caring website. It has helped me a lot. I am improving with your suggestions of stretches and am now at 118 degrees 3 wks after MUA and PT 5x wk. It has been a long and painful road so far. Could you tell me what I should expect going forward? How long it will take and what I can hope my knee to get back to? Besides the pain, the not knowing is really messing with my emotions. 3/4/2019 07:10:41 am
I am pleased to hear that this website has been helpful to you.
Reply
Nancy
2/27/2019 01:25:23 am
I had tkr right knee in July 2017, no problems with the surgery, not much pain through any of it. Went back to work as a florist in 3 months. Lots of standing, lifting, bending, walking, heavy work. Still no pain but just in the last few months the swelling is horrible. I come from work and can hardly walk. My surgeon took x rays and everything looked good, my flexion is good and my bend is 120. I need to have my left knee done soon but not sure if I want to go ahead with it if my right knee is so swollen all the time. Wondering why the stiffness and swelling is getting worse. Thank you for any comments.
Reply
2/27/2019 10:05:09 pm
Swelling without trauma in a knee replacement that had been functioning properly is concerning.
Reply
Brenda
3/15/2019 07:30:50 pm
Hello,
Reply
5/12/2019 10:56:51 am
My experience is that manipulation needs to be done within 8 weeks of surgery. Beyond this point the soft tissue contractors/scar tissue will not yield to a reasonable force.
Reply
Neil Coleman
4/6/2019 05:53:31 pm
I am 66 yrs old , and I am fit and active . I had TKR 11 months ago , for arthritus . After 6months I had 0 deg. ext and 95deg .flex , and was making good progress . I was playing social doubles tennis , but not quite able to road bike . Generally feeling positive , back at gym and doing regular stretching exercises . 8 months post.op , I had discomfort in knee , with swelling and heat . Had to ease off on physical activity . Weight bearing after sitting was a problem , as well as a very clicky knee . I revisited my surgeon who x-rayed and declared the new joint "pristine " but suggested there had been some tissue damage , and keep up the exercise . My Physio has given me specific quad strengthening work , and I am currently using your excellent "flexing with strap" regime to increase my flex to about 100deg . I also have regular massage , and have been taking low dose antiflam medication.
Reply
5/12/2019 11:13:01 am
It sounds like you have a bit less range of motion than would be ideal for your desired level of activity.
Reply
Surgery for complete left knee replacement March 6, 2019. The first 2 weeks I did the recommended physio at home. After the two weeks I started physio up to the day before I saw my surgeon at 7 weeks. I’ve been to pt 12 times. Very and extremely painful every time. Since the fourth week I have felt a piercing hook on the left side every step I make, preventing me from doing them properly. As a result, it makes me afraid of what i will feel when my foot touch the floor.
Reply
4/30/2019 08:29:41 pm
I am sorry, I do not understand what is meany by a "cup hook." If you can clarify this in other words, perhaps I can help.
Reply
Jo
6/26/2019 08:03:15 am
10 months post total knee replacement. I have at least 115 bend and completely straight leg but I still have an awful tight feeling across the top of my knee when walking. I'm hoping it will wear off in time??
Reply
7/22/2019 08:31:52 pm
Following total knee replacement, your body will lay down new, thicker scar tissue. This may feel stiff for a long time. Although this tissue will always be present, it should gradually loosen up for a long time. Additionally, the lateral aspect of the knee (outside aspect) is often partly numb, this can feel abnormal, some may describe this as "stiff." With the range of motion you have achieved, I would expect you to feel better and better as months go by.
Reply
1/16/2021 08:26:03 pm
I’m 4 months out from TKR. 65 yrs old male 150 Ibs. Knee flex 0 to 115 with help 120. I still have swelling real bad painful stiffness across knee where meniscus once was. Similar to what others mention, riding stationary bike to warm it up helps before I stretch for a hour. I can’t stand on it for longer then 15 minutes at a time. I can walk heal to toe on it with minor limp but painful after 20 minutes. Doctor had recent CT scan showing implant was aligned perfectly and no other issues appears to be scar tissue getting worst daily due thickening. Did a allergy study for metal and came back negative. Do you recommend I have the lysis arthroscopic surgery with MUA at this point? 1/16/2021 09:17:58 pm
@John Cranias:
Nancy B
7/17/2019 11:00:31 pm
Hi Dr G, I am still recovering from a patella fracture on Nov 2018.
Reply
7/22/2019 08:39:30 pm
Outstanding job on regaining motion! Unfortunately, after a fracture, your knee may never feel perfect. It is common to find the hardware used to repair the fracture irritating, and I would expect improvement in symptoms once this is removed.
Reply
Nancy B
9/1/2019 06:25:54 pm
Hi Dr G
Reply
9/1/2019 11:26:13 pm
I am glad to hear you are feeling well. I think doing unweighted long arc quad exercises is fine to help regain full, active extension. I would definitely not recommend adding weight to this exercise though, as it could rapidly become irritating to your patella. And yes, I would recommend avoiding open chain strengthening forever. Single leg squat/leg press are better ways to strengthen.
Reply
9/2/2019 03:47:04 am
I broke my knee June 10th-fell on tile. Only hurt initially. I never had any swelling or mobility issue the 1st week. Was doing everything I normally do-including mowing my lawn with zero pain or problems. All my problems started when I fnd out I broke my knee 1 week later. And i only fnd this out. Because my GP sugg. I have it x-ray since i had broke a toe 10 days prior-and was going to Ortho to have that X-rayd. Found out broke my Patella. but Orthopedist sd it was in a good place. But if I would continue to bend it. I could possibly end up needing surgery. Since it should stay straight for 6 weeks to heal. ALL MY PROBLEMS started with the immobilization. I had horrible calf, ankle, and foot swelling. i got numbness, and my leg felt like glue was poured in there. This went on for 6 weeks. I was so uncomfortable -I called ask-a nurse 2 nights. I was told to go to ER.Since calf swelling could be blood clot. Waited till Monday-told my GP this. He tells me i don't have a blood clot. I sd how do you know. He says " I'm a Dr?" He agreed on my request to let me have ultrasound referral. Where blood clot was ruled out. But this continued. And 2 weeks later when I called Orthopedist upset.They recommended another Ultrasound. Where blood clot ruled out agn. Nothing else was ever suggested from my Orthopedist or GP for these symptoms. The immobilizer came off July 28-6 weeks from June 17th. 6 weeks of hell. When it came off- i asked the Orthopedist. " Is this swelling going to go away?" He says maybe? I had 2 physical therapy sessions. But I couldn't get more than 95 degree bend in the end. Due to my calf and behind knee swelling. Another P therapist told me I wouldn't till I got rid of the edema. So-here i am now-more than 1 month from immobilizer off. I am able to get enough rom to ride my recumbant road bike now-but that's it. And I've only ridden it 3x for about 10 min-because when i get off-10 min later-my lower leg feels worse than ever-stiff cement like. Numbness comes and goes. My ankle when I try to move it-feels like I'm trying to move burnt skin. A lot of the swelling has gone. But I still have some. I can't lift my right foot off the floor more than about 10 inches. And I can't safely walk my 2 big dogs. I'm not walking totally normal by any means. I have taught aerobics a good part of my life. And I happen to be very flxible. My left foot-at 65-I can still put to my mouth. And bend back and touch my butt easily. My right foot now. I can get facing a wall. I'm 1/2 way to the butt-that is a lot of lost rom. And I feel horrible-between the 3 symptoms. Do you suggest-static stretches for me also? I use the neighbors pool. And when i 1st get there. My calf is hard as a rock. I'm able to get fluidity to it in about 10 min. But after the 50- 60 min I'm there moving. As soon as I get home-20 min later-It's BACK-the stiffness. Tuesday I have an appointment with a chiropractor for a compression boot session. And last week I had the grad-forget correct spelling technique done by him. Not so sure that was a good thing. Felt fine agn for 15 min-stiffness back 15-20 min later. And the procedure painful. Common sense tells me pressing on my leg with a stainless steel instrument-to get fluid moving-may not be the best method. So- I need advice. I'm getting very depressed about all this, I feel half crippled from a simple break that required no surgery. Chiropractor sd i should have been offered massage during this 6 weeks of immobilization-to keep fluids moving. And I'm wondering if a brace that allowed minimal movement rather than none. Would have been much more common sensical. Now my patella is healed -But I'm half crippled?
Reply
9/16/2019 08:19:44 pm
Rehabilitation after a fracture can be frustrating. I would expect progress for an entire year of more following a patella fracture. Nonoperative treatment of a patella fracture does require immobilization. Now that you are healed, it is important to have patience and persistence. You should be stretching progressively every day. The stretching I recommend on this website for patients following total knee replacement will work for you as well.
Reply
Verna Lister
9/16/2019 08:44:50 am
I had a TKR on Aug 15, 2019. Prior to TKR I had only a maximum of 93 degrees flexon due to prior injuries. Total tears in 1988 to ACL and i 2009 PCL..some Medal lateral damage, After 4 weeks post op of have about 80 degrees flexon, extension seems OK. What should I expect by 6 weeks and what should I do for stretching?
Reply
9/16/2019 08:09:02 pm
In my opinion, you are a bit behind schedule in regaining your range of motion. My experience suggests it is very unlikely for patients to predictably regain much flexion beyond 6 weeks from surgery. I recommend long duration, slow steady stretching, as often as possible, for as long as possible.
Reply
Verna Lister
9/30/2019 09:08:29 pm
I have been doing to prolonged stretches and making more progress. But to add further information for your consideration. My knee flexon was a maximum 0f 93 degrees for more than 4.5 years prior to surgery..so how would this change the rom by 6 weeks? Would further ROM and more weeks bring a more acceptable ie 115 degrees? I am seeing surgeon Wed. I will advise him of my progress. Any further incites to why I am experiencing lack of rom to date? I have done stretches and PT every day?
Reply
9/30/2019 09:16:59 pm
Poor range of motion prior to surgery definitely correlates with a more challenging rehabilitation process after surgery. This is in spite of the surgeon regaining full, unrestricted, range of motion at the time of surgery. It appears you are now around 6 weeks from surgery. In my practice, if you are still stuck around 90 degrees at this stage, I would recommend undergoing manipulation under anesthesia. This usually makes a huge difference for patients.
Reply
Patrick Shipley
10/3/2019 12:58:07 am
Hello,
Reply
10/7/2019 08:22:38 pm
Hopefully you are trying to stretch the way I recommend in this article. My experience with stiff knees really suggests that short, rapid stretches are ineffective. Check out the article I wrote on viscoelasticity.
Reply
Patrick Shipley
10/3/2019 01:38:09 am
I’m sorry, I had my weeks messed up. My Manipulation procedure was on August 22nd which was 11 weeks from my total knee replacement surgery June 4th, 2019.
Reply
Brenda Solomon
10/6/2019 05:12:50 pm
I had knee replacement surgery three months ago. My range of motion is good 126. I have completed PT. Now I use my stationary bike daily and try taking long walks. But my knee can still feel very stiff some days especially after standing or walking for long stretches. Does this stiffness eventually go away? Is there something else I should be doing? Everyone says it takes awhile. They told me that Medicare will not pay for more PT.
Reply
10/7/2019 08:08:34 pm
From my perspective you are doing great for this stage. While every patient has a somewhat unique experience following knee replacement surgery, I would expect stiffness to gradually improve for a whole year. At this stage I recommend progressively resuming your desired activities. It is ok to use ice if the knee gets swollen or sore. Be confident that the way your knee feels at 3 months is far from the final product. Congratulations on your excellent early rehabilitation.
Reply
Amy T Lake
3/10/2020 04:30:35 pm
I had total knee oct. 2016 and then may 2017. It is now 2020 they still hurt when I stand 4 or more hours. Is this normal? Can they still swell even though the parts aren't bone? Some days they feel as big as boulders in the inside, but can't tell on the outside. I work 40 hrs a week medical assistant. I had them rechecked and had to pay big money for all the x rays but I'm still not convinced. 3/11/2020 10:21:55 pm
It is not normal for total knee replacements to hurt as you describe. I can take a while for a patient to recover enough to stand for several hours at a time. If your knees swell, it is not the metal prosthesis or bone that is bigger, it is extra fluid contained within the knee joint. This fluid is made by the synovial tissue inside the knee. This is living tissue. I usually remove most of this tissue at the time of surgery, but not all surgeons do. Some patients will have recurrent swelling after knee replacement. This does require some investigation beyond simple X-rays if the swelling and discomfort are significant. Sometimes blood work is necessary. Sometimes additional radiographic testing is needed. Perhaps you should consider a second opinion if you are not satisfied with the explanation you were given by your surgeon. 10/10/2019 10:32:10 am
Keep up the great work! Thank you so much for sharing a great posts.
Reply
10/14/2019 06:17:47 pm
It is my pleasure! I am glad to hear that you enjoy this website.
Reply
Jim
10/12/2019 03:45:01 pm
I had bilateral tkr sept 5/19 and found your question and answers very helpful, thank you so much for doing this.
Reply
10/14/2019 06:16:16 pm
I am glad to hear you find this site helpful, thank you for the feedback!
Reply
Christine
10/18/2019 02:17:44 pm
I had a total knee replacement over 4 years ago and had very little pain and recovered very quickly. The only slight issue was a small area of tightness on the outside of my leg just above my knee
Reply
10/28/2019 07:20:51 pm
It sounds like the combination of heavy shoes that fit loosely probably required more energy to walk. I would recommend supportive, properly fitting shoewear.
Reply
Abinesh Jegatheesan
11/19/2019 10:23:36 am
Hey I had broke my lateral femoral condyle in a freak accident in April. After the internal fixation procedure I struggled a lot with my range of motion and my knee became extremely stiff and it was recommended that I undergo arthroscopic treatment to remove the scar tissue. I had that done last week on November 8th. Ever since I have been on my CPM machine, consistently doing my post op exercises, going to PT, but there hasn’t been much change in my ROM. My knee is still quite swollen, but I’m still quite discouraged with my progress so far. Is there anything I can do to improve my ROM?
Reply
Terry
11/22/2019 02:47:47 pm
I am a 65 year old female who had a total knee replacement 3 weeks and 3 days ago. My flexion is 115 and the leg lies flat. I have the tight band sensation people are talking about. I am incredibly thankful I found your information and will begin the stretching exercises, holding the leg for some time, rather than seconds. Your information has given me peace of mind that I am doing okay, and has answered SO many questions I’ve had. I sincerely cannot thank you enough for taking the time to answer so many questions. Thank you.
Reply
11/22/2019 11:04:58 pm
I am glad you find this website helpful. It sounds like your total knee rehabilitation is right on track - your range of motion is perfect for this stage.
Reply
Sandy Perna
8/26/2020 10:24:00 am
This is me to a tee! I’m so discouraged with this tightness, which no one gave me straight answers about. I am actually 4 weeks post op and will now start the exercises mentioned here and hope it’s not too late.!
Reply
8/26/2020 07:41:46 pm
It is definitely not too late. Just keep stretching every day for long periods, and you should see progress.
joyce stein
12/26/2019 02:13:38 pm
I am 5 and 1/2 months out from total knee replacement. I have good range of motion. Can't do stairs due to clunking and pain behind knee. I go to the gym every other day for strengthening exercises and recumbent bike. Can go upstairs fine no pain. Catching young clunking going downstairs. Mild clunking when I walk. Can minimize it if I keep my glutes tight while walking. He does get irritated from all this clunking. Wondering if there is any exercises that would minimize this. My Doctor says he could replace the plastic in my prosthesis with a different kind if I'm still having a lot of trouble in 3 months.
Reply
1/11/2020 10:22:53 am
This probably deserves an entire article, but I will attempt to answer your question briefly here. A total knee replacement is a mechanical device made of hard materials (metal and plastic). A variety of motions are possible between these components. Because the materials are hard, mechanical sensations are common and often quite normal and anticipated. A properly balanced knee will not have major catching and clunking, however. Severe clunking can indicate synovial tissue becoming caught between components, ligament imbalance, or mechanical debris caught between the moving prosthetic components. Exercises are not likely going to help. The fact that your surgeon suggested a polyethylene plastic exchange suggests that he/she is concerned about ligament instability. I would also suggest getting a second opinion from another surgeon before committing to a revision surgery.
Reply
Jason Hancock
1/16/2020 07:36:23 pm
I'm a 47 year old man and I'm 9 days post op. I am really struggling like most with flexion and I'm currently at 90° my physiotherapist is making me go a little beyond what I can handle pain wise with her help and holding only 5 seconds. My progress seems to be creeping along and feel like this is brutality! Lol. My question is, when you say to hold these exercises longer using minutes instead of seconds, do I have to be at a point of almost agony when I hold? Or can it be a bit less so I can prolong the exercise? As I'm typing this I'm thinking the answer may be obvious! Thank you!!
Reply
1/17/2020 10:46:34 am
This is a very common question. The problem is that when you force range of motion for just a few seconds, your tight muscles will spasm and even the biggest, strongest physical therapist in the world will be unable to move your knee. Particularly at 9 days, there has not been enough healing yet to create any significant "scar tissue" that physical therapists love to talk about.
Reply
Jason Hancock
1/17/2020 12:07:23 pm
Thank you so much for your quick response! My my therapist just left and I have achieved 97° which is a 7° improvement in 2 days. I definitely see that the morning PT is easier than the afternoon which I assume is because of less swelling and pain due to 8-10 hrs of rest. Thanks again. 1/25/2020 08:34:39 pm
I had my R TKR on June 5th 2019 and at 6 weeks was bending great, don't know the degree, but about half way up my thigh. I had my L TKR on Aug 5th and bending was the same. I was cut loose from PT that was done at home. I am 60 years old. I was a 5 day a week tennis player and am in good shape, not overweight and wondered why it has become so still.Seemed to be doing great but my R knee started getting stiff. I've tried ride the recumbent bike, but I know it's not bending as well as it should. I seem to be able to rotate but my right ankle is bending funny to accommodate the rotation. Now, on the Right side I can only bend it to the top of my calf. The Left (second surgery) still bends like it's supposed to. I can straighten them both flat. I called my ortho office and it's taking 3 weeks to get in for a appt. They both click when I walk. I have no problem walking. Just the Right bending. I've been trying to work with it but it's really not budging much at all. I've tried soaking in epsom salts and then stretching but I can't tell that it's helped at all. It's quite frustrating. I had rotator cuff repair in Dec of 2018 to repair 3 tears and it healed quite well without any scar tissue. Do you have any idea why the first surgery has adhesion's? I would appreciate any advice. Thank you so much, Cami Gorsky
Reply
2/1/2020 12:59:51 pm
Unfortunately, I do not have enough information to answer the question (why your right knee got stiff after "bending great" at 6 weeks.) I agree that this is not typical. Usually once rehabilitated, a normal knee replacement is expected to easily maintain functional range of motion for decades without having to constantly dedicate time to stretching.
Reply
Gordon Fitzsimmons
1/31/2020 07:37:47 pm
Hi, I am pleased to have found your site and have spent time tonight reading through the posts and answers/advice given. I am particularly interested in the references to "tight", "tight band". I am 9 months post tkr on my right leg and 6 on my right. Of the two, my right has been more of a success to date. I have had a fair bit of I believe soft tissue issues with my right knee/leg . Thankfully this is settling down a bit. I have good ROM and straight legs; I followed my PT program and was discharged from my sessions and returned to work after a few months. What concerns me is this tightness/stiffness above both knees (lower quad/quad tendon). I can walk on the flat and go up hills (with slight awareness of it), use my excercise bike also, however walking down gradients/slopes is a problem. I feel I have to take baby steps due to this tight band/concrete band feeling above my knee. I have even at times gone down slopes sideways as it's much easier. My daughter thinks it's equivalent to a woman walking down hill in high heels. I feel I'm going to fall face down at times. I'm currently trying to take longer strides , but the tightness persists. Is this the scar tissue you refer to ? If so will this go away/settle down given more time ...I'm approaching 1 yr post op in April. I continue to do excercises given to me by my PT back last summer. I will try the longer stretches you mention. Thanks in advance for any advice on this.
Reply
2/1/2020 12:53:22 pm
You do not specify your range of motion, other than "good." I assume this to mean 120 degrees or so. I think your difficulty going down slopes is more likely due to relative leg weakness and should improve with time and strengthening of your hips, quadriceps, and hamstrings. There are some technical issues with regard to knee replacement design that can make them somewhat less forgiving going down hill. It is very important to work on strengthening to help you with this. This being said, I recommend that everyone avoid open chain quadriceps exercises (quadriceps extension machine) and instead focus on squats, lunges, etc. I hope this helps you.
Reply
Gordon Fitzsimmons
2/3/2020 03:42:42 pm
Thanks for allowing and responding to my post. Your advice is much appreciated .
Julie High
2/7/2020 09:39:01 pm
Hi. I am a 60y/o female post LTKR December 18, 2019. Two weeks post-op my ROM was 117/0 and 125/0 at 6 weeks. I've had extreme nerve pain that stings, burns and becomes achey. That started about week 3 and I was told that sensitivity was normal and would go away. I started doing desensitization and the nerve pain was starting to subside at around 5 weeks.. I saw my surgeon at 6 weeks, 5 days and everything looked good. Prosthesis fit was good, x-ray looked good. I discussed the desensitizing with my Dr. and how the nerve pain was starting to subside. We also talked about using Palmer's cocoa butter over the incision site and massaging to break up scar tissue. I did that with his go ahead and I don't know if I massaged too deep but something has changed. I feel stiffness, like a band is being held over my knee. I have almost constant nerve pain, whereas before it only occurred late evening. I also feel a cord shape (vein?) palpable under the skin that extends mid-knee horizontally to the lateral side of my leg that ends at the bend. I've been actively involved in my PT before surgery and post-operatively without any issues. I was unable to complete full reps of my exercises yesterday because of the pain. Today I went for therapy and my PT did light massage, some light exercises and gentle movement of my knee. I'm so frustrated because everything seemed good, with the exception of the nerve pain which was actually resolving until I massaged my scar with the cocoa butter. It seems like it was a simple thing to do. Now I'm concerned that something has gone wrong. This new pain is excruciating and wearing me down. Thank you for your time.
Reply
2/8/2020 06:29:17 pm
I think you are only experiencing the normal thickening of the soft tissues around the knee as the healing process progresses. Scar tissue tends to toughen and contract over time. Ice, massage, stretching and (most importantly) time should take care of most of the sensitivity and tightness. As always, if there has been significant deterioration in your knee's appearance and/or function- have your surgeon check it out in person. Excruciating pain is not typical for this stage in your rehab.
Reply
Lindsay
2/21/2020 08:56:14 pm
Hi there. I'm a 29 year old female, and I broke the distal head of my femur within my left knee playing soccer 11 years ago which appears to have healed nicely without surgery. Years later, I had increasing pain and last year an orthopedic surgeon found that I had significant wear and tear on the inside of that patella with some bone loss. About 10 weeks ago, I had a osteochondral allograft transplant from a donor placed onto the kneecap. PT was terrible after that due to a combination of problems (bad post-op pain that started PT off for about 5 days, a physical therapist who was too aggressive and never did the type of PT you've talked about on here, and the possibility that I scar quickly). Anyways, I could only get about 70 degree flexion with no progress for four weeks. So I had to have scar tissue removal surgery at 9 weeks (9 days ago) and my surgeon said I had extensive adhesions all over the place that were virtually "cementing" my knee down. He got 135 degree flexion during manual manipulation under anesthesia. After this surgery, my surgeon wanted 90 degrees flexion 3 days post-op, but I could only get about 40 and apparently my patella was already very stiff at that time. Right now on my CPM and at physical therapy, I can get to about 65 degrees with a lot of tension and pain. And my kneecap feels more stiff than last week. My thigh muscle and perhaps tendons/ligaments above my knee are insanely tight and feel so much pain when stretched. I have done well to learn to relax during PT and I'm even on valium and opioids to try to continue to relax these muscles. I know I could bend my knee more if these muscles would stop being so tight. They hardly feel like muscle anymore. And while I simply try to bend my knee outside of an actual PT session, these muscles are like tightropes and the knee bends maybe 15 degrees.
Reply
3/6/2020 02:34:30 pm
Unfortunately, I am unable to state why, exactly, you have become so stiff. It does happen sometimes. It is called arthrofibrosis. Some patients have a very difficult time relaxing into the stretch. If the response to pain is clenching the muscles, then stretching becomes very frustrating. The best thing to do is to be very gentle with the stretching, but to hold the stretches for a very long time. This allows the muscles to fatigue, and relax. Use some pain medication and ice or heat while stretching. Try to distract yourself during the stretch. Stretch for hours everyday, with no days off. Your hard work will pay off.
Reply
Mita Vyas
3/2/2020 02:37:26 pm
Hi Doc,
Reply
3/6/2020 02:26:11 pm
It is possible to improve your range of motion for up to a year from surgery. This will take dedicated time and effort on your part. I would argue that 125 degrees of flexion is an excellent result, and should allow you to do just about anything necessary for a happy life. If there is a particular reason you need more flexion, then keep stretching, but if it is simply to get a "better" number, then I think you may have more pleasant things to do with your time.
Reply
Tonya
3/6/2020 04:41:50 am
Hello,
Reply
3/6/2020 02:23:04 pm
I understand your reluctance to undergo more surgery. A manipulation is generally done using only IV sedation, and no incision is made. This usually must be done within 6-8 weeks of surgery for a reasonable chance of success.
Reply
Tonya
3/8/2020 09:06:13 am
Thank you so much for responding!
Bill
3/25/2020 09:00:00 pm
Stats - Age 67 , TKR Oct 15 , MUA Dec 16 , Current ROM 90 (95) . Can you explain why it was necessary to perform MUA before week 8 vs your thinking of Long Duration Stretching even after a MUA has been completed . I thought that after week 8 or 9 the contras had formed and the only way to remove scar tissue was more surgery ?
Reply
3/25/2020 10:49:08 pm
After surgery scar tissue begins forming. This scar tissue becomes more robust over time. Early range of motion exercises are very important to regain a functional range of motion before this scar tissue becomes so dense that it will not yield to stretching exercises. Within 6-8 weeks this scar tissue can be gradually elongated by stretching it. It is dose dependent- meaning the longer the stretch is held, the more effective it will be.
Reply
Matt B
4/6/2020 10:53:41 pm
Hey Doctor! Thanks for all the replies I’ve found them very helpful. I had surgery on my left knee February 11th, 2020 for my MCL (repair) and to remove Osgood Schlatters build up that had been causing me irritation. The Doctor who did my surgery put me in a knee immobilizer after the surgery for 4 weeks keeping my leg completely straight. I then started PT and my knee was completely stiff and could only bend about 5 degrees. The most we’ve seen it bend in therapy has been 65 degrees, but this is with they Physical Therapist pushing it down. Really 55-60 degrees is what we get it to by the end of our therapy session. I’ve now been in therapy for 4-5 weeks (3 days a week) and have been putting in the work to stretch it at home. I saw the Doctor again today and he was angry at the PT’s advising they weren’t being aggressive enough, although I’m yelling in my therapy sessions from the pain. He advised we may have to do another surgery due to the stiffness. Any advice for me? I’ve just started doing your recommended lengthy stretching sessions and will continue doing this daily. Thanks. Appreciate you and could really use the help.
Reply
4/16/2020 03:36:22 pm
The best bet for a very stiff knee is long duration stretching, as often as possible, for as long as possible. This is best done passively- meaning that you should not have to use any muscle strength to force the stretch to happen. You should try to relax your entire body while stretching. Ask your surgeon to consider a static stretching brace- for example - Joint Active Systems.
Reply
Eli Joseph
4/13/2020 12:10:04 pm
Hey Dr. G!
Reply
4/16/2020 03:41:31 pm
You do not quantify what you mean by "substantially worse," but I assume this to mean worse than 120 degrees of flexion. I would think you should be able to regain a decent range of motion on your own since you had excellent range of motion just a couple of months ago. I recommend focusing on long duration stretching, as often as possible, every day, for as long as you can tolerate. Try to make these stretches passive- meaning you should find a way to stretch that allows you to relax your entire body during the stretch. I demonstrate a variety of examples of this throughout this website. I doubt another MUA will be needed if you really dedicate yourself to a stretching regimen.
Reply
Gloria Applegate
4/26/2020 08:38:15 pm
I am a 60 year old woman. October 28, 2019 (basically 6 months ago) I had double total knee replacement surgery because of severe pain from arthritis. I was in the hospital 4 days, then entered inpatient rehab for about 4.5 weeks. I had physical therapy each day from the day after surgery until i left rehab, with great therapists who worked on extension and flexion and strengthening. My left leg did remarkably better than the right, from the very beginning. After I returned home, I had home health come by for several weeks to guide me through home exercises until I could get into an outpatient PT facility after the first of the year. I was in PT there from January through March, usually 3 times a week. All in all, I was in therapy from November to March. At end of therapy my left leg was approx 120 degrees and my right 110 degrees, with a bit of help from therapists to get to that amount. I have not had a great amount of pain through any of this but what has remained consistent is the amount of numbness and stiffness and the tightness that comes after a workout, in both legs, although more on the right than the left. My surgeon always has my legs xrayed at each visit and says they look great. He quickly asks me to show him my extension and flexion to which he says it looks good and to my complaint about the constant stiffness he merely says that recovery can take up to a year and I am coming along normally. I feel that he is not taking my concerns seriously as he is in and out of the room in under 3 minutes and is rather dismissive. My PT feels they have done about all they can for me and I am able to continue my work on my own. I have no complaints about the therapy I have received as I believe they have been thorough and taken the time to work on many aspects with me. However, they don't have any real explanations on why I continue to have numbness and stiffness when walking, sitting too long or after a good workout. I am reminded over and over that its only been 6 months and I can expect the healing to continue for up to a year. My hope is that they are all correct. During these 6 months since surgery I have been diligent and worked hard at therapy and done exercises and stretching at home as recommended. Since therapy ended however I have not been doing nearly as much. I hoped that taking a break might allow my body to rest and recuperate and heal and that the stiffness/tightness across my knees might recede. It has not. The past 4 days I have been walking and doing stairs consistently. It doesn't seem to have changed anything either. I have spent the afternoon reading through posts like your's, in hopes of finding out what I am missing and/or doing wrong. I am beginning to worry that I will have this tightness from now on and that i will have to learn to live with it. Any insight or help you can give me would be most appreciated. TIA.
Reply
4/27/2020 08:44:35 pm
I think the advice you have been given sounds correct. I understand you would like your surgeon to spend more time with you (this is a common issue) but, there is really not much your surgeon can do for you now. It is not unusual for the knee to feel stiff or sore for many months after surgery. And most people DO report improvement for up to an entire year. It is hard to be patient, but time is on your side.
Reply
Gloria Applegate
4/28/2020 09:14:56 pm
I appreciate your timely response. Would doing the long duration flexion and extension exercises you speak of on this website be useful in my situation? If so, do you have a page or site that I could look at that explains/pictures all the recommended exercises? 5/11/2020 07:02:30 pm
This is a good article to start with. Right in the beginning you will find several helpful links.
Theophilous Ebenehi
5/7/2020 06:08:04 am
Hey Dr G!
Reply
5/11/2020 06:59:30 pm
When someone loses range of motion in their knee, this requires investigation. I recommend you see an orthopedic surgeon in the office. They will examine your knee and obtain X-rays. At 19, without trauma, these x-rays are expected to be normal. If this expectation is correct, and MRI is needed to rule out a displaced meniscal tear or loose body (which is a free-floating piece of bone or cartilage) that can get caught in the joint.
Reply
pat costello
5/13/2020 02:39:54 pm
hi doctor 8 weeks ago i had surgery on my knee for a complete tear of the quadriceps from the knee cap im in a brace since but last week i was to my surgeon & he let off the brace down to 110 which is fully off but he said to keep it on when walking i got excercise to do at home but one of them is to try & bring the knee back where it should be but it will only come a small bit as its very tight on the knee cap & the muscles at back of knee are very tight i dont wan to force too much in case i tear the tendon off the knee again regards pat
Reply
5/18/2020 07:17:37 pm
It sounds like your surgeon has made appropriate recommendations for this stage of your recovery. I would expect you to gradually regain range of motion for up to an entire year following surgery. If you have 110 degrees already, I think you are doing quite well.
Reply
Pat costello
5/19/2020 11:39:25 am
Thanks very much for your reply regards pat
Kevin Cheyne
5/22/2020 05:51:29 pm
Good Afternoon Dr Gorczynski
Reply
5/26/2020 07:57:26 pm
I definitely think long duration stretching is the way to go. Clicking can have a variety of causes and it is not possible to be definitive in your case via the internet. If it is associated with swelling, the kneecap may float up a bit when your knee is extended and then engage into the trochlear groove in the femur with further flexion. You may experience this as a click. This is just a thought. If this is indeed the cause, it will resolve with time, as your swelling improves. Anti-inflammatory medication and/or ice will also help with pain and inflammation. And, look forward to many months of gradual improvement yet to come.
Reply
Julie Mittman
6/10/2020 06:35:17 am
I had a TKR on 25/3/2020.I have had trouble walking as there seems to be something catching on the bottom outside of my knee.I am able to to all the non weight bearing exercises and my bend is 118%and 1% off straight When I have to push with my toes it catches and really hurts.Also when I wake up I can't weight bear at all and this is painful to start to walk as all the muscles especially the outer ones right up to the top of my thigh are extremely stiff
Reply
6/26/2020 06:54:11 am
This complaint should be investigated by your surgeon. Your range of motion is totally acceptable, and compatible with an excellent, pain-free result. While some pain, and stiffness is normal for a couple of months following knee replacement surgery, this should be trending down, particularly at 3 months from surgery. While you are far from maximum improvement (which can take up to an entire year from surgery) inability to bear weight at 3 months from surgery is clearly not normal. I recommend you contact your surgeon for an examination and x-ray evaluation of your knee replacement.
Reply
Viola
6/29/2020 01:29:06 pm
Six months after total knee replacement and still have stiffness and difficulty bending or walking. Tested on blood for everything including metal allegories and all come back normal. I can (with 20-30minutes of exercise) increase ROM, but lose it again after walking a short distance. Had a manipulation at 3 months and this caused no difference. Any suggestions?
Reply
7/1/2020 07:27:14 am
In my experience, manipulation at 3 months is very unlikely to be effective. I recommend manipulation at 6-8 weeks. Beyond this, a stiff knee usually requires arthroscopic lysis of adhesions in addition to the manipulation. Even then, there is not a guarantee range of motion will easily return as this procedure is being performed in a high-risk individual. At this point, I would discuss this procedure with your surgeon.
Reply
Viola
7/1/2020 11:46:10 am
Thank you for your quick reply. I’ve been doing your long stretching since first reading this blog. How is it possible for me to gain ROM to almost 140 after about 45 minutes of stretching, and then lose it again? After a short time, it is painful to bend beyond 90 degrees and I must start over again. Could something have shifted (tendons or ligaments since X-ray is good for replacement), could it be scar tissue or could my immune system be the problem by causing inflammation? Taking Celebrex, but have taken myself off of Tramadol. 7/1/2020 09:35:17 pm
If you are able to achieve 140 degrees of flexion while stretching at 6 months from surgery, and your surgeon feels your x-rays look good, I would be patient, continue stretching, and let time pass. I would expect gradual improvement for up to an entire year after surgery. Particularly since you had a relatively recent manipulation- you are still within a significant inflammatory period of recovery. If you tolerate it, consider using some anti-inflammatory medication and definitely ice your knee after stretching- these modalities should help reduce inflammation.
Reply
I so wish I’d found this site sooner! I’m 7 weeks out of TKR and am at 108 degrees bend. I’m concerned that this not good enough. My Dr. mentioned manipulation but because I was able to get from 90 to 108 in two weeks (A time frame he gave me) he said I didn’t need to. My knee is stiff but not incredibly painful at least not like before. Do you think prolonged stretching would help me? I’ve never been told to do that. As a few people have mentioned here this surgery has really affected me mentally. I don’t know if I could go through the pain and even more therapy of a manipulation. 7/26/2020 10:43:15 pm
@Keely - 108 degrees is not "enough," but I agree with your surgeon. You have achieved a functional range of motion, and gained nearly 20 degrees in 2 weeks time. I believe, with solid effort, daily stretching, and generous use of ice you will probably gain at least another 10 or so degrees over the next month. I definitely recommend prolonged stretching, particularly at this stage of your recovery as the scar tissue is starting to become more organized and stiff. Check out my article on viscoelasticity which explains this further.
Andy
8/10/2020 07:15:10 am
I had a TKR las Wednesday (august 5th), so far all seems to be ok. 2 questions: 1. very stiff on my upper hamstring - halfway between my hip and knee. I have not seen any comments/reference to that. this seems to be preventing more knee flexion. any comments please? 2. I would swear I hear feel movement of the muscles/knee when I move (like clicking but not quite that pronounced, just feels like muscles/knee is moving a bit). is this normal? I do understand that the muscles around the knee were stretched back some during surgery. would appreciate input here as well. thank you.
Reply
8/14/2020 05:36:17 am
It is still very common for surgeons to use a tourniquet during surgery. If this was the case, some bruising and/or soreness around your mid-upper thigh is frequently seen and will rapidly improve. While it may be sore, when stretching properly, it should not hinder your ability to rehabilitate adequately.
Reply
Andy
9/4/2020 10:28:48 am
Dr. Gorczynski - thank you very much for your reply and apologizes it took me so long to say thank you. as I am now exactly one month, I am improving steadily, and I will say some of the pain in making progress is substantial. With that said, everyday the swelling seems to be getting better and mobility improving.
Christine
8/31/2020 12:14:41 pm
I am 3 months post TKR surgery. Since the beginning of my PT I have been wearing a thigh-high compression stocking. My physical therapist recommended it and says my swelling has gone down rapidly as a result of wearing it during the day. The stocking also reduces the “clicking” In my knee; the feeling of “metal” in my knee; and reduces the pain. Is there any reason for me to discontinue wearing the stocking? Will it affect the healing process?
Reply
9/3/2020 05:14:06 pm
As long as your wound is healing nicely, and you do not mind taking the stocking on and off for hygiene, I see no reason you should not continue using it. Keeping swelling down is definitely encouraged. It should not harm the healing process.
Reply
andy
9/9/2020 10:00:10 am
Dr. Gorczynski, again thank you. I would like to ask 2 followups. 1. I am now 5 weeks post op and I still have swelling on the top of the knee. its almost like a 2" wide / 6" long band of swelling that follows under the scar. Is there anything I can be doing to help accelerate the swelling going away? 2. When I push my flexing (at about 105 degrees) I get a serious stabbing pain on the underside / outside of the knee that prevents further flexion. Any suggestions on how to break thru? I am doing all of my suggested PT everyday. thank you. Andy
Reply
9/10/2020 03:22:34 pm
It is normal to experience some ongoing swelling at this stage for recovery after knee replacement. Ice, gentle, long duration stretching, and time will all contribute to its gradual resolution.
Reply
andy
9/12/2020 07:52:48 am
Thank you very much for your quick response.
Christine
9/12/2020 05:58:40 pm
My TKR was 4 months ago. From the beginning I have had the sensation (on the outside part of the knee) of something catching and/or not operating smoothly. In the last month it’s gotten worse. It frequently happens when I change positions on bed. When it happens I have to stretch my knee out for it to feel normal again. I don’t see my Dr for another month. Should I see him now. For the first 2 months i made incredible progress—all the PTs were amazed. Now I feel like I have regressed. I do have more pain than I had at the earlier stage especially sitting down and standing up. Thanks for your help.
Reply
9/13/2020 10:48:54 am
Without knowing your knee's range of motion, it is hard for me to make much of a recommendation. As I discuss elsewhere in this blog, there are several moving parts inside your knee (with or without knee replacement surgery). This could cause mechanical sensations. That being said, it is not common for a patient to experience a catching sensation that worsens with time. If you have a concern, definitely see your surgeon sooner than scheduled. To be clear, some mechanical sensations can be normal, some pain can still be normal at this stage, and I would expect improvement in knee function and pain level for up to a year or more following knee replacement surgery.
Reply
Chris B
9/12/2020 10:39:25 pm
Good evening - I had my left knee replaced 15 months ago. Things went well. Good range of motion. No pain. Tonight I noticed a "wobbly" bit on top of my knee cap, closer to the inside of my leg. If I press on it, it shifts. It feels quite hard (ie, not a squishy lump) Is this something I should be getting checked out or maybe it was always there and I never noticed it before? Thanks in advance for your advice.
Reply
9/13/2020 10:22:28 am
In the absence of pain, and as long as it isn't getting larger, or red, it probably does not require any significant treatment. As always, there is no harm in having your surgeon check it out at some point. I would recommend setting up an appointment at your convenience. Things that would suggest more urgent evaluation is needed include: fevers, chills, increasing pain, increasing redness, loss of range of motion. As long as these things are not happening, it is probably some scar tissue, or calcified adipose fat) tissue, neither of which require treatment.
Reply
Chris B
9/13/2020 10:29:52 am
thank you for your reply. I'll keep an eye on it and follow your advice.
Alicia Erickson
9/18/2020 01:28:54 pm
I am 52 and had a total knee replacement 10 weeks ago. My flexion is up to 127 and my got my extension to 0. I have been doing the stretches you mentioned everyday. I am still experiencing a lot of stiffness, especially during the night. I am still swelling quite a bit after activity. I mainly ride my bicycle on a trainer inside and do my stretching exercises. I am still doing PT 3x a week to help with the stiffness. When I am stiff I walk with a limp. After PT or stretching my walk improves then it all starts over again the next morning. Just wondering if this is due to scar tissue build up that I still need to work through and wondering how long the stiffness could potentially last? Also wondering if I am doing all the right things? Stretching, PT, and icing constantly. Thank you!
Reply
9/20/2020 02:35:57 pm
Your range of motion is excellent. I would recommend you maintain your exercises, use ice /anti-inflammatory medications for relief as needed. At this stage after knee replacement, your body simply needs to heal. As long as you maintain your range of motion, as time passes, the inflammatory process will gradually wind down. I would expect continued improvement for up to a year or more following knee replacement surgery.
Reply
Hello I am 3 and a half months post up TKR. I started working again and I stand like 3 hours in the a.m. And evening is about 4 to 5 hrs. I am not in any pain but it feels a bit odd in the kbee. I do ice when I get home. Is it okay to be standing this long after a TKR.
Reply
9/22/2020 09:21:17 pm
As long as you are not experiencing any pain, your knee does not swell up, and you do not lose any range of motion, I think it is OK to be back working at this stage following knee replacement surgery.
Reply
Becky
9/23/2020 08:12:38 pm
I had ORIF surgery after a fractured patella on 7/21/20. I can bend my knee to 125 degrees by doing a heel slide or just bending my lower leg back. But when walking my knee stiffness and swelling won’t let me bend back very far. I can walk fine with a bit of a limp. When I walk with the injured leg the knee sort of bounces the lower leg back too soon. Would that be solved with the knee stretches you described above? I’ve been mostly doing quads exercises so far. It seems like if the problem was adhesions I wouldn’t be able to get 125 degrees ever. Hope you can help me understand how to address this.
Reply
9/23/2020 08:36:54 pm
With flexion to 125 degrees, this does not appear to be a problem with adhesions. You do not specifically state it, but I assume you have full extension. It sounds to me that you have some residual gait abnormality that will resolve with time and work with physical therapy. If you have weakness with bending- instead of focusing only on quad exercises, add hamstring exercises. Also check out my article on anterior knee pain- those exercises should be very helpful to you.
Reply
10/8/2020 02:24:33 pm
Looks like one of your knees still needs a little work on extension. The other one looks well rehabilitated. I would recommend working on the prone hang technique on the knee that does not go fully straight.
Reply
Many thanks for answering my questions. Wanted to clarify one more item with the extension and flexion. Since I have met my goals with the flexion do I need to continue my PT exercises I am doing at home to maintain 120 and 121? The same question for the knee that I achieved 0 for flexion. 10/15/2020 04:34:23 pm
While it never hurts to do some gentle, long duration stretches, at this point (over 3 months from surgery) it is unlikely to result in significantly more range of motion. At this point, I see no reason you should need to spend several hours working on exercises every day. Perhaps take a few minutes each day to stretch simply to make sure your knee range of motion is maintained. Then, maintain whatever physical activities you enjoy. Rest assured that your knee is expected to feel better and better for months yet to come. 10/7/2020 03:00:50 am
Great blog.thanks for the share.<a href=https://boneandjointcare.co.in/>Knee Surgeon In Mulund</a>
Reply
Shelley
10/12/2020 04:47:47 pm
Had a PKR 6 weeks ago. Have bend at 130 degrees which is great. Been doing exercises and stretches routinely each day. However went for a long walk 3 days ago (45 minutes and browsing the shops for 2 hrs) and how pain in inner knee area and some swelling again (had none prior). Worried I've done something to the knee which has damaged or is it telling me to stop the long walk? BTW thanks for the blog so encouraging reading.
Reply
10/15/2020 04:28:56 pm
It sounds like you have overdone it a bit. While this is likely just irritation, if you are now having pain with weightbearing, I suggest you ask your surgeon to examine your knee, and perhaps also obtain new x-rays. Although unlikely, new pain with weight bearing that results after nearly 3 hours of weight bearing activity soon after partial knee replacement could indicate a stress fracture. Pain with weightbearing in this situation should not be ignored.
Reply
Andy Monshaw
10/16/2020 02:06:49 pm
Dr. Gorczynski - first, I would like to thank you. I have remain subscribed and find everyones Q&A to be helpful and informative. This is the only place I have found to have this level of discrete information, and its clear we are all concerned for a complete recovery.
Reply
10/24/2020 04:09:25 pm
It sounds like your iliotibial band may be inflamed as it crosses your femur or the prosthesis on the outside of your knee. As you have observed, this is not commonly discussed. It is a fairly common question for patients to ask at around this stage in recovery though. I would expect this to gradually improve with time. It is very unusual for this pain to persist.
Reply
Andy
10/24/2020 06:06:26 pm
thank you. 10/20/2020 01:03:24 am
video would help to see therapy flexion and straightening exercises
Reply
10/24/2020 04:15:27 pm
Thanks for the suggestion. I am currently working on some longer format video, as I agree that it would be helpful. In the meantime, check out some video clips on how to use a yoga strap to help regain range of motion after knee replacement.
Reply
Sylvia Hubbard
10/20/2020 04:14:12 pm
Dr. G, I am 16 weeks post TKR when I completed my 12 visits of therapy my flex of my knee was at 128 and I could straighten my leg fully. I have no pain, but still dealing with stiffness when I have to sit for a period of time. Don’t remember this stiffness with my right knee TKR but that was 5 years ago and I’m73. I have no problem with walking.
Reply
10/24/2020 04:11:50 pm
It is very common to experience stiffness after a period of inactivity at this stage following total knee replacement. It will improve with time. Sounds like you have regained an excellent range of motion. Nicely done!
Reply
MM
11/2/2020 02:29:07 pm
Today I am 6 weeks post op TKR right Knee. My flexion is 90 degrees and extension is approximately -8 deg. I am still in PT 2X per week and continue to do PT exercises at home. My knee is stiff too. I am glad I found your site and advice concerning stretching.
Reply
11/8/2020 08:06:10 pm
Unfortunately you are starting to run out of time to regain range of motion. Definitely spend as much time as possible stretching to try and catch up. Hopefully you have a follow-up appointment with your surgeon soon. I think it is appropriate to discuss possible manipulation under anesthesia so you can regain a functional range of motion. Best wishes!
Reply
Hello,
Reply
11/26/2020 02:05:30 pm
I am concerned about the possibility of ongoing, low-grade infection based on your history and complaints. The classic findings of fever, redness, and swelling do not necessarily have to be present for low virulence infection to be present.
Reply
Uma
11/12/2020 01:12:17 am
I underwent open surgery for pvns 6 weeks ago. Synovectomy was done and tumor removed. I started physiotherapy 4 weeks ago. My flexion is around 90 degrees.
Reply
11/26/2020 01:59:12 pm
You absolutely have enough time to regain full functional range of motion after a procedure like this. The stretching exercises and techniques I recommend are perfectly applicable to you. Best of luck!
Reply
Uma
11/28/2020 10:16:04 am
Thank you so much for assuaging my doubts. I have been distressed that I was unable to attain full rom at the 6 week mark that is applicable to TKR patients. 11/28/2020 01:42:47 pm
Just continue with long, slow end-point stretching. Try to do this multiple times every day. Use ice/NSAIDS (if you tolerate them) to reduce inflammation. I would expect you would be able to improve your range of motion for many more months to come. Best of luck, and keep up the good work!
Reply
Uma
11/12/2020 01:18:40 am
Just to add I'm 36 years old and in good health.
Reply
Sharon
11/12/2020 12:40:47 pm
53F 5 weeks out frim TKR. Flexion <50 Extension 0. MUA scheduled at six weeks on the dot. What should I do for therapy in order to have the highest chance for increased ROM after MUA. Include X10 and/or Dynasplint? Thank you!
Reply
11/26/2020 09:25:22 pm
The best recommendations I have are in articles throughout this website. The summary is: get to the endpoint and hold it for as long as possible, as often as possible, and take zero days off until you achieve your goal for range of motion.
Reply
Barbara Mcintyre
11/19/2020 03:12:06 am
Hi Dr G, I’m 69 yrs old had right TKR 3 yrs ago left TKR 2 yrs ago. Recovery has been normal for both knees & have been doing great. Recently got a stationary bike & ride 25 min low resistance & walk few times a week. Wish I was more active, it’s hard with the pandemic. Although I have occasional clicking in knee on & off but infrequent. But about 2 weeks ago noticed crunching feeling ( no pain at all) in knee when getting up from sitting.its happened a few times. Now area around knee feels tighter, heavier. It’s not red & minimal swelling. I thought I’d give the bike a break. Maybe that was irritating knee. I really don’t stretch at all. I’m willing to do anything you recommend. Thankyou, Barb
Reply
11/26/2020 09:30:16 pm
It sounds like you have developed some synovitis (inflammation of the joint lining). Perhaps a bit of rest is appropriate. Make sure you have a couple rest days each week, particularly after a more strenuous workout. I would also recommend using some ice, which will help reduce inflammation. Consider adjusting the seat on your stationary bike a bit, make sure the seat is high enough, and positioned not too far forward. Make sure your feet are not being forced into an abnormal position if you use clipless pedals.
Reply
12/7/2020 08:51:08 pm
I recommend long duration stretches.Typically physical therapists do not focus on LONG duration stretching the way I do throughout this website. Take a look at the "ALL ARTICLES" section of this website, There are several articles addressing how I recommend rehabilitating a knee replacement. Additionally, I recommend using ice, and anti-inflammatory medications if you can tolerate them.
Reply
Hello, I’m a 55 year old retired army vet. I injured my knees during my time in the service. Ii has surgery on 20 October so I’m at my 8th week of a total knee replacement recovery. I’ve had a DVT in my calf which was discovered during my post-op appointment. It’s still there after 6 weeks. I had the self injections of medicine (blood thinners) into my abdomen first then they put me on another blood thinner (pills) since and it’s still there.
Reply
12/22/2020 11:25:12 pm
It sounds like you have had a tough time....Based on your progress thus far I think at this stage manipulation is appropriate. Your surgeon should be able to get you caught back up to a reasonable level of flexion (110-120) if this is done soon. If you decide to proceed in that manner, I would strongly advise focusing on stretching as your full time job for several weeks afterward. Use ice and anti-inflammatory medications if you can tolerate them. Spend hours each day stretching.
Reply
Collins
12/24/2020 08:40:56 am
Reading ur reply have been helpful of previous comment,you are truly the best, I had im nailing of my tibia on both legs and the incision was from my knee down, my left leg perfect post op,didn't don't any exercise and I regained full range of motion 3weeks post up, did the right tibia op a month after the first and I am in 3rd week now,started PT daily after 2weeks bcus of swelling,I can do every stretch and extension except touching my heels on my but when I lie with my stomach faced down,its soo painful on the right side of the knee when I try full extension to touch my heel on my butt,sharp pain when I try to push down and hold,what she'd I do to be able to touch the heel on my butt and is it normal to have this knee pain during tibia operation(intramedullary nailing)
Reply
12/24/2020 10:33:36 pm
Anterior knee pain is not uncommon following intramedullary nailing as the insertion point is just behind the patellar tendon (just under your kneecap). This is a sensitive area. Scar tissue can make this very sensitive area tight and stiff postoperatively. I would be patient with your knee. In my opinion, you have at least 6-8 more weeks to regain range of motion, possibly even longer. This surgery is much more forgiving relative to knee replacement surgery as there is much less trauma within the knee joint itself. Just follow your surgeon's and therapists advice and work on daily stretching exercises. This plus time should maximize your recovery.
Reply
12/27/2020 09:23:09 pm
I would hold the stretch for several minutes at a time, minimum. Longer if your knee is stiff. Ideally, you will have at least 0-90 degrees motion by 2 weeks post-op, 0-120 by 6 weeks post-op. If you are not making progress quickly enough to meet these benchmarks, add more stretching duration, and additional stretching sessions.
Reply
Moira Spearman
12/29/2020 08:40:33 pm
Hi, I’m 10 weeks post op and had 95 degrees bend when I left hospital at 4 weeks post op I was 120 degrees.
Reply
12/29/2020 09:32:44 pm
At only 10 weeks post-op you are far from fully recovered. Count on continued improvement for many months yet to come. Just keep doing your exercises. If you are able to maintain 0-120 range of motion at this point- simply maintain this and allow your body to heal.
Reply
1/3/2021 12:32:40 pm
Hi Dr. Gorczynski,
Reply
1/4/2021 09:28:13 pm
You only have a few degrees to go to regain full extension. Are you doing prone hangs? If not, I think you should try. Spend increased time working on this technique daily, and I think you still have a decent chance of gaining full extension.
Reply
John K.
1/4/2021 09:26:24 pm
Dr G. I am glad I found your website. I am 66 years old and just completed the 10th week from TKR. I did PT the first 6 weeks and have continued the exercises daily at home. I had 120 degrees deflection at week 4 but things kind of stayed there. My P Therapist and doctor did not say much about stretching it further. The last 2 weeks or so after reading your blog, I have stretched it a lot and I am now at about 130 degrees but with pain when i get there. I am doing the stretching every day along with the exercises and riding my stationary bike for an hour. Do you think I can improve beyond 130 degrees ? if so what do you think is the max I can get to ? also how long before the soreness on the knee goes away ? thanks a lot.
Reply
1/4/2021 10:18:02 pm
It sounds like you have adequate range of motion for your desired activities. If this is the case, then I would recommend against forcing your knee to bend more simply to gain bragging rights.
Reply
Trey Wilson
1/5/2021 06:33:10 pm
Hello, my name is Trey and I am 33 years old. I underwent ORIF to my right patella for a slip and fall on 11/12/2020. My ortho recommended not bending my knee and had me in a circular cast for 4 weeks. Once removed he had me in a leg immobilized with full extension for 2 more weeks. Now I am 7 weeks post op and only have about 70° of flexion. I am cleared to start PT but my ortho is recommending manipulation under anesthesia. I do not want to go forward with the procedure at this time but he has given me until this next Monday to make a decision before he will not offer it for me anymore. I am currently uninsured and money is an issue in these difficult times. Would your method of hanging my leg over the couch arm be beneficial for someone in my position or would you recommend I have the MUA? If I am unable to have the MUA would your methods help me gain any range of motion at all? He stated that I should still be able to gain a few degrees but it wouldn’t be very significant without causing much pain. Thank you for your time and looking forward to hearing from you.
Reply
1/5/2021 10:37:13 pm
You were treated appropriately after this procedure. Based your range of motion, it is reasonable to consider manipulation at this point. There is a time window, after which manipulation will not be effective. I agree with your surgeon, if you are going to undergo manipulation, it should be done prior to 8 weeks postop.
Reply
Jennifer
1/8/2021 09:34:20 pm
I had a tto, mpfl implant, outer tendon release, and a macy on 11/4. I was up to 90 degrees at 6 weeks when we discovered a wound infection. The wound doctor had me stop all pt and strengthening for past 2 weeks. I was released to start again yesterday. I immediately started walking. I cannot however move past 40 degrees now. It is very painful behind my knee. Could it just be stiffness from disuse these past weeks, should I be worried, and any tips to move or help the pain behind so I can push back to 90 degrees? Any advice is helpful.
Reply
1/16/2021 09:23:43 pm
Long duration stretching. I wish there was another secret I could share. I do have some videos demonstrating how I would stretch on my youtube channel:
Reply
Simon
2/26/2021 01:49:55 am
I had knee surgery 6 weeks ago, but have not yet seen a physio face-to-face because of the pandemic lockdown in my area. Yesterday I went for a follow-up appointment with the surgeon and he said I may have come off my crutches too early (4 - 5 week) and that he'd expect me to bend more by now.
Reply
3/12/2021 02:41:31 pm
It is not typical to require crutches at all after knee replacement. Slight shift in implant position is possible early after knee replacement (particularly when using a press-fit/non-cemented) prosthesis. As long as it stabilizes and you become pain-free- no problem. Stretching is much more important than doing squats or strengthening. This is because regaining motion is unlikely after 6 weeks postop. Strength will improve for many months/years.
Reply
Abdou Mbacke
3/10/2021 01:38:04 am
Hello, I am 20 years old and have done an OATS procedure on my left knee on January 15 2021. After 6 weeks my range of motion was only 25 degrees so we did a manipulation. It has now been 1 week and a half since my manipulation and I can go up to 120 degrees on the cpm machine with pain and 90 degrees without. On my first physical therapy session I went up to 98 degrees of flexion. However on my second session I went down to 90 degrees and now my range of motion is slightly worse. I am scared that my knee flexion will get worse. What should I do? And with all due respect please be very specific. Thank you in advance.
Reply
3/12/2021 02:18:33 pm
Stretching for long durations as I describe on this website and on my videos is as specific as I can be. I am not withholding any special moves. Gently, progressively, make your knee move. Try to relax as much as possible while doing so, so that you are not just fighting against your tight muscles.
Reply
Donna
3/21/2021 03:43:27 pm
I am 62 yrs old and 11 wks from tkr on left leg. First 6 wks went well. 120+ flexion with no problem. Got extension from 15 to 6-7 by week 6 but can’t seem to get better than 6 no matter how hard I work. Dr says I should be able to get it resolved with another 2 weeks of the intensive therapy I have been doing for the past 4 wks. I don’t want to limp and use a cane forever. Also have very stiff knee after sitting for any more than 20 mins. Dr does not believe MUA will help. Should I keep pressing for a resolution or settle with what I have?
Reply
3/28/2021 11:18:40 am
I would recommend you keep working to achieve full extension. The prone hang technique is fairly powerful. Perhaps also ask your surgeon for a static extension stretching brace. This might help you hold the stretches for longer periods.
Reply
KKimbrel
3/29/2021 11:50:10 pm
I’m 57 years old , I’m almost 7 weeks post op from a partial knee replacement , it was on the interior part of my knee . My flexion is 125 and extension is 1. I’ve been disciplined when it comes to the stretches and moving the knee . I work the leg/knee daily and I cycle over an hour a day with moderate resistance . My concern is the same as many others . I feel like I have a rock for a knee and the extremely painful tight band feeling . I’m still confused , is this swelling/inflammation or a tight tendon or an issue with a ligament . It gets unbearable early in the evening . My hopes are to return to work at week 10 ( truck driver ) can you please help me understand this unbearable feeling of having a brick for a knee being held in place by extremely tight bands . Thank you for this site , it has helped so much .
Reply
4/13/2021 07:42:28 pm
At only 2 month from surgery, you are very early in the healing process. You will improve for an entire year. Keep stretching, use ice and NSAIDs if you can tolerate them. Let your body heal and be patient with it. This is one of the most challenging operations to recover from. Your motion is excellent- just maintain and trust your body will make excellent progress for many months. Cycling daily with resistance could be somewhat irritating to your knee at this stage. I would consider this optional right now. If you choose to continue cycling- use ice afterward to help reduce the resulting inflammation.
Reply
Nancy Zahul
4/14/2021 06:59:26 pm
Hi. I have gotten TKR on both of my knees. I'm at 6 months on the first knee with flexion at 115 and extension at 5. I'm at 4 months on the second knee with flexion at 113 and extension at 8. I can walk and bike without pain. However, I'm not yet walking at the speed I was able to walk 5 years ago and not biking as far as I was able to bike 5 years ago. I have trouble doing squats and going down the stairs. I can go up the stairs, but slower than a normal person would. My main problem is stiffness after sitting for more than 20-30 minutes. I don't feel stiffness when I'm sitting. I only feel it when I stand up. When I stand up, my knees are really stiff and it takes me about 25-30 steps before I can walk like a more normal person and without the stiffness. I'm curious to know whether the stiffness I feel when going from sitting to standing is normal at the month I'm at on each knee. Is this kind of stiffness due to not having 120+ flexion or do I just need to be more patient? Since Saturday, I've been doing the legs up the wall exercise displayed in your video. I've been doing this every day, four times a day. I bring my feet down until it's very uncomfortable and hold for 15 minutes. I have a REALLY hard time getting my bent legs out of this position and into a straight-leg position. It really hurts. I'm curious to know whether this is normal. Should I keep doing the legs up the wall exercise or is it hopeless? I thank you in advance for answering my questions.
Reply
4/25/2021 10:30:04 pm
I am more concerned about the flexion contractures you describe. (you are unable to fully extend either knee) This position results in an abnormal gait and increases the pressure between your patella and femur. This will present as anterior knee pain, worse on stairs/hills/squatting. Take a look at the prone hang technique I describe. While there is no reason to stop working on flexion, I would prioritize extension.
Reply
Lynn D
4/21/2021 12:52:59 pm
I wish I would have found this blog last year. A fall in March 5,2020 caused a patella fracture that required surgery to wire but the lower third had shattered so I had reattachment of the lower tendon. Was in an immobilizer for 10 weeks. After 10 weeks of therapy, one hour, 3 times a week I regained 95% bend while sitting but lost range of motion. Even after a year I have difficulty with stairs, can’t put a shoe on my right foot without assistance, and still can’t drive. I’m 5ft tall and the angle of car seats makes my knee hurt. My ortho recommended walking and said “enjoy your life, just don’t fall”. Should I seek another round of therapy?
Reply
4/25/2021 10:12:24 pm
More therapy certainly won't hurt. Perhaps follow-up with your surgeon is appropriate for a re-evaluation. If your motion is poor at this point, perhaps you can discuss arthroscopic lysis of adhesions with manipulation.
Reply
Bridget
4/27/2021 03:06:49 am
I'm 8 months out trkr I never made it past 100 degree and I'm about 3 in being straight..
Reply
5/11/2021 05:09:42 pm
Unfortunatlely, in my experience, it is unlikely a patient will be able to regain much motion without surgery when they only have 100 degrees of flexion at 3 months postop.
Reply
Darrel Donatto
5/14/2021 05:13:40 pm
A simple thank you for the excellent information and videos. My knee replacement is 10 days out and I found the information you are providing helpful.
Reply
Michael Matthews
5/27/2021 05:56:37 pm
My TKR was 12 weeks ago. Beginning 1 wk Post-Op, I did PT 3x/wk for 11 wks. Since 3 weeks Post-Op I've been swimming 5x/wk for 40 min each day (in retrospect, I'm hoping that swimming mitigated scar tissue development). Now I'm trying to get more than 120° and -3°ext at home. Do you think it's possible?
Reply
6/23/2021 10:40:18 pm
It is definitely possible for everyone to get this range of motion after total knee replacement. Swimming does not require much knee motion though, so this alone will not do it. Stretching on a daily basis as I describe throughout this website is the way. You don't state your current range of motion, so it is impossible for me to gauge you progress thus far. Generally after 6 weeks post-op gaining more motion is increasingly difficult. It is for this reason I created this website. The sooner after surgery you regain motion, the better.
Reply
Mike
6/9/2021 04:54:12 pm
I'm about 10 weeks out of post op from two meniscus repairs, acl reconstruction (patellar graft) and mcl reattachment back to tibia in my right knee. I went into surgery about 10 days after my basketball injury that caused this issue. I'm getting to around 115 of flexion on my own but need help from my PT to get me to 120. I feel like I've been stuck around 115-120 for the last 3 weeks. I do get to extension at 0 but if I focus on my flexion stretches too much I have to work to get back to extension. Then I start focusing on extension and get it back to 0 and my flexion goes ROM goes down. Do you think my flexion range of motion still open up over time? I'm about 20-30 degrees short of my normal leg flexion. I haven't taken a single day off from stretches and I started therapy the second day after my surgery. I'm really trying to avoid another surgery at this point. Have you seen knees open up over the year as swelling goes down or is it really hard after 10 weeks.
Reply
6/23/2021 09:01:35 pm
I would expect you to gradually regain range of motion for up to an entire year following the surgery you underwent. This is quite different from total knee replacement. My best advice is to continue doing what you have been doing, with long duration stretching on your own every day in addition to PT. Hold the stretches for minutes not seconds. Try to get to a cumulative hour at the endpoint every day.
Reply
Mayank Patel
8/24/2021 07:21:43 pm
Hello- just following up. So I actually just had lysis of adhesions and MUA 4.5 months after my previous mcl(reattachment) acl and both menisci reconstruction. I was struggling with extension (+5) and flexion (105 active and 115-120 with PT stretching). It’s been 7 days since the second surgery and My knee extension is perfect now -I’m at 0 but am still struggling with flexion. Im still stuck in the 105-115 range 7 days after surgery? Should I be concerned? Everytime we push my knee to 115-120 I feel like my knee swells up and I go backwards in flexion. Will the knee open up naturally over time with continuous exercise? I’m really trying to get all my ROM back in these next 6-8 weeks.
Trish
6/16/2021 12:38:35 pm
I had an orif of my right because of tibial plateau fracture on the medial side and ligament rapture, it’s now been 5weeks post operation and I’m still at 70degrees flexion and no extension, please what can you recommend for me
Reply
6/23/2021 08:53:07 pm
You generally have more time following trauma/trauma surgery to regain range of motion compared to total knee replacement surgery. I would just stretch for long durations as recommended throughout this website. If your progress is too slow, consider asking your surgeon for a JAS or similar progressive static splint to help.
Reply
Roger Spink
6/27/2021 09:59:24 pm
Hi Dr G
Reply
6/28/2021 12:28:41 pm
It is unusual to lose range of motion as you describe. While I definitely advise stretching for long durations, I would also encourage your to follow up with your surgeon to make sure the prosthesis is ok, and to discuss options.
Reply
Tammy Smith
7/5/2021 04:00:44 pm
Hi,
Reply
7/28/2021 08:30:48 pm
This sounds like a very reasonable approach in your specific case. As always, I recommend slow sustained stretches for the best, least inflammatory motion gains. Best of luck to you!
Reply
Daphne Palmer
7/8/2021 09:46:08 pm
I am 8 months post left TKR and my range of motion is excellent. But I still have pain that is present mostly with standing or sitting for long periods. The pain feels like a tight band around my knee. I would rate it as a 5/10 at its worst. The only thing that helps is lying down. This has not improved in the past 2 months. There is no swelling or tenderness. My surgeon was not worried about it. I just had my first session today with a new PT who feels it is muscular and is doing a lot of deep focused massage/manipulation. I also just ordered a TENS unit. Ibuprofen 600 mg does not help. Question: Is this normal and will it improve eventually?
Reply
7/28/2021 08:26:58 pm
While this is not typical for a knee replacement at this stage of recovery, everyone is a little different, and some patients report significant progress with regard to motion, pain, swelling, and stiffness for a year or more following surgery.
Reply
J Croteau
7/28/2021 11:47:11 pm
Arthroscopic surgery to remove debris in 1989 but hole identified in cartilage. Cartilage repair 1990 (deep coring to encourage bone and cartilage growth) and a repair in 1998 followed by TKA May 2019 at age 58. Physio daily (2x per week in clinic), daily exercises per recovery instructions. Use of CPM to keep bend at 110 (loss of range nightly). By end of July 2019 needed MUA as loss of flexion continued. By July 2021 flexion 85 and went to see surgeon. Surgeon looked at xrays and knee alignment is good but stiff knee and loss of range due to scar tissue from multiple surgeries. It seems to me that scar tissue grows back quickly. Is it worth it to get scar tissue removed?
Reply
8/19/2021 04:37:29 pm
Removal of scar tissue alone will not be helpful. You would need arthroscopic lysis of adhesions followed by manipulation under anesthesia. This means the tight tissues that form between your quadriceps tendon/extensor retinaculum and the femur need to be cut, then your knee needs to be pushed through a full range of motion. This procedure alone is not curative. It provides another opportunity for you to rehabilitate your knee, hopefully using different tactics this time. Poor rehabilitation following this procedure will leave you in the same position you are in now. Stretching for long durations as outlined throughout this website is the most effective way I have found to regain range of motion. With only 85 degrees flexion, it is definitely reasonable to consider this procedure, but it is crucial that you rehabilitate differently that you did the previous time. In my experience CPM is useless in a situation like yours since it really only helps midrange motion. You must force your knee to bend, even if it hurts.
Reply
J Croteau
8/19/2021 09:27:11 pm
Rehab was very aggressive for all previous surgeries so there was never ever poor rehab. CPM was used only after MUA two months following TKA due to loss of flexion overnight and only used at night. Used CPM after original bone surgery, immediately in Recovery room until hospital release 5 days later to excellent results, so thought it would help at night after TKA. Got to 110 after TKA then lost gradually each night eventhough diligent and enduring pain during the day. I felt like I was loosing whatever gains I was making daily during overnight. Working with physio now to try to get back to 90.
Ken S
8/7/2021 07:02:06 pm
Dr. Gorczynski,
Reply
8/19/2021 04:22:13 pm
You are getting to the stage in recovery where additional gains in motion are less likely, and take much more effort to achieve. The good news is that you have regained a functional range of motion. As time goes by, the tightness is expected to gradually resolve.
Reply
8/23/2021 10:22:37 pm
My sister's knees were severely damaged due to the sport she's playing, which is why she has decided to start looking for the right surgeon that may address the matter. Thank you for sharing here as well that tissue pains will be opened during the procedure. It's also a good thing that you clarified here the possibility for scar tissue.
Reply
Kellie
8/25/2021 08:17:39 pm
I had MPFL reconstruction w/donor ligament and arthroscopic loose cartilage removal after an injury to my left knee. Unfortunately I injured my right knee When I was 12 years old and I have lived my life relying on my left leg due to recurrent subluxations in right knee. And It is an understatement to say that my body has learned to protect my right knee at all costs Now, this has become huge factor in my rehab of my left knee. My biggest challenge is extreme fear and protection ingrained in my muscles and brain transferring to my left knee. I am finding it extremely difficult to allow my knee to bend. My physical therapist has to do massaging and really force knee bend every time. He says the majority of that is due to my apprehension and subsequent contraction of my upper leg muscles when I feel any pain or fear that I’m going to dislocate my kneecap even though he assures me that that won’t happen because I had the repair done and This leg this knee is not the same as other knee. I am five weeks post surgery and with extreme struggle at every session we are only able to get to 74° of flexion. Without using force I can get to about 40° of flexion on my own but it hurts. I’m getting really frustrated because i really don’t know how to make my body stop involuntarily protecting via tightening my thigh muscles. Logic and reason do not seem to work here. Please help.
Reply
9/1/2021 04:06:46 am
Increase your duration of stretch. Use ice to reduce inflammation. Perhaps consider asking your surgeon for medication to help reduce anxiety (like valium) to be used while stretching.
Reply
8/30/2021 08:42:03 pm
I had total knee replacement on right knee in February 2021. My ROM was 95 degree before surgery. Surgeon and physical therapist had goal for me to reach 95 degrees after surgery. I was in a brace for four weeks after surgery due to stretched ligament. I could bend 45 degrees at two weeks and then brace was removed at four weeks. I wen to PT for over two months. I am in no pain now and have no stiffness. However 95 degrees is pretty limited and my goal of being after to walk down stairs normally has not really been realized. I had/have knock knees and limited ROM for years. I'm getting left knee done next month. Is there any chance that ROM will improve beyond what you had going in to surgery?
Reply
9/1/2021 03:17:19 am
While it is true that (in general) a stiff knee prior to surgery will make regaining motion after surgery more challenging, it is definitely possible to regain more motion than you had prior to surgery. It sounds like the bracing that was required after your surgery has led to your difficulty with range of motion. Hopefully this will not be required for your next knee replacement.
Reply
Trish G
9/2/2021 08:59:01 am
I wanted to send a kudos for this blog topic. I'm 17 days post op and doing great with 110 degree passive ROM so far. The sofa with legs dangling is exactly what I need and I feel this will be an immense help to my daily PT sessions. Already have done this and can feel almost immediate improvement in my morning stiffness. Just wanted to send a thanks, no need to publish.
Reply
Judith Woods Sloan
9/14/2021 08:50:14 am
I am 5 weeks out of TKR of my left knee. Knee flexion yesterday was 124. However, my left ankle has begun to be quite painful when flexing my knee. My left foot has always turned in, and still does. As the PT was measuring for flexion at one point, she was making sure my foot was straight and the pain was awful. Is this normal? The PT said we can work on my ankle and she wasn't worried, but I heard a "yet" in her facial expression.
Reply
10/5/2021 03:41:49 pm
This is not normal. Particularly at over 5 weeks from surgery. If this continues you should see your surgeon for examination and x-ray. Amongst a variety of possible explanations, you may have arthritis in your ankle that has gotten irritated by the surgery or rehab, or could have developed a stress fracture as a result of changed mechanical axis of your knee following surgery.
Reply
Kathleen
9/15/2021 03:24:53 pm
To give hope to anyone doing a TKR -- I am 60yrs BMI 39 , 5'10" female and at 5 weeks after TKR and have achieved 132degrees bend , amazing , no pain . and I do 3 times a week PT and do the explained work out daily ... I used the prescribed automatic machine in bed at home first 14 days to move my leg and bend 5 hours a day . The first 12 days achieved 120degrees . By the first follow up I was 125 degrees and the surgeon and I was extremely happy .Best part , NO PAIN , No Narco drugs and only NSAIDs . I do have to say ICE is the best friend , all day long and self PT keep moving. Using a Clutch while driving freed up my Patella . week 4 back to work with cane , week 5 walking no cane , can walk up stairs , get off toilet , go up curbs . Only taking a OTC Tylenol . I wish everyone great success after TKR as my life before was like a root canal every time I stood up ..
Reply
Maggie Paraiso
10/3/2021 11:10:37 am
I had TKR August 2, 2021. I have been going to PT since August 5. My ROM is still at 100 and ext.at 2. My Ortho Doctor informed me to consider MUA in two weeks. I do not know what to do at this time because, my ROM had been slowly going up. I had a bad case of stiff leg prior to surgery, with very low ROM, which made me decide to get surgery done. My right knee is to be operated on next. I will appreciate hearing advice from you. I am 75 year old “nana”.
Reply
10/5/2021 03:12:45 pm
If you were my patient, I would encourage you to consider MUA if you haven't gotten beyond 100 degrees by 6 weeks postop. The problem is that it becomes increasingly difficult to achieve more motion as time goes on. This means that the range of motion patients have at 6 weeks is what they will end up with. In your case, 100 degrees is suboptimal. It is not totally unacceptable, but much less than typical, and could interfere with good function/pain relief. If you wait significantly longer, then the success of manipulation decreases and it is much more likely an invasive procedure (arthroscopic lysis of adhesions) will be needed prior to manipulation. There is significantly more risk involved with this.
Reply
Nancy T
11/26/2021 06:44:19 pm
Thank you again for taking the time to help so many people. I am in week 8 of a tkr on my right knee. ROM is 0 - 130. I can wait there and walk and up until a week ago I could do 20 minutes of biking on a recumbent bike. However my PT switched my exercises to more weight-bearing and stair stepping and during a stair stepping exercise a sharp pain went through my l outer knee and down to my ankle. I had to stop and ice. Coincidentally I was seeing my surgeon for a last post-op visit. I hobbled in with an ice pack stopped my knee but he saw saw nothing functionally wrong and thinks it might be scar tissue.However the pain has persisted for the past week and a half, particularly when I twist the leg, such as getting in and out of the car. I have to hold my knee in my hands to do any quadriceps exercise.. No loss in range of motion and swelling is minimal. I can walk without assistance but it is a little stiff and painful to push through with my toes. I take one meloxicam in the morning and Tylenol as needed. Will stretching help this? Do I need to worry or just give it time? Any exercises to avoid? Should I keep trying new recumbent bike? I can stand on the way just fine and balance. It is very perplexing.
Reply
12/16/2021 04:09:24 pm
Hopefully by now your knee has improved and you are back on track. If you continue to have pain radiating from your knee to your ankle, this is not normal. You really need a more specific diagnosis than "scar tissue" before any guidance can be given. You seem to have excellent range of motion. If your pain level has not improved, and X-rays are normal, perhaps your surgeon could consider obtaining a metal artifact reducing MRI scan to evaluate soft tissues, and rule out stress fracture adjacent to the implant.
Reply
Diana Allingham Rubanenko
11/28/2021 09:06:42 am
I’m a woman of 73, 3 weeks post-TKR and found your wonderful site yesterday, searching for solutions to stiff knee. Wow! what an encouraging experience. Your altruism in helping people who may never become your patients (I live on a different continent, for example) is so unusual, and your replies are totally informed and professional, yet soothing at the same time. I showed your site to my PT who came for a last home visit today, he was very interested and then took me for a too-long walk and up and down flights of stairs in my apartment building. The after-care facility where he works believes more in functional physio that features with lots of walking, he says. The fact is that I only felt better after getting home and getting back to stretching as you recommend – (started yesterday with a total of 20 minutes and will get back on track tomorrow). Thank you so much!
Reply
Pushpa K
12/30/2021 12:15:13 pm
Hello Dr,
Reply
1/22/2022 01:30:59 pm
This is a knee that would be a candidate for manipulation vs. arthroscopic capsular release followed by manipulation. This is a discussion to have with your surgeon. I typically manipulate around 6-8 weeks when needed. Once a patient gets beyond 12 weeks, I think arthroscopic release followed by manipulation produces better results.
Reply
1/17/2022 11:21:07 am
Hi Dr Gorczynski,
Reply
1/22/2022 01:16:44 pm
I would definitely get on the waiting list for the other total knee now, since it will be years to actually get this done. I am blown away that this kind of waiting list is acceptable in your country. Our current throughput is severely restricted due to COVID, so now our patients have to wait 12 weeks, and while they are quite understanding, also find this wait barely tolerable.
Reply
1/24/2022 06:18:39 am
Thank you for the advice, I will give a shoe lift a go. I am doing some IT band exercises to release that tension down the side but the knee still feels as if it is in a vice being squeezed. The UK waiting list is the government says about 5 million for operations, some other outlets are saying realistically it is about 12 million! who knows the true figure. The issue is during covid they basically stopped all surgeries, they estimate at least 50,000 cancer cases have gone undiagnosed. This is what happens when you focus only on covid. 2/26/2022 03:34:48 pm
You make some very legitimate points. If there is some way for you to have your surgery in the United States, it would be done within a couple of months.
Reply
Tammi Cotter
1/18/2022 01:55:40 pm
Hello! I am not sure how I found this website but so glad I did. I too have stiffness (I am 15 weeks post-surgery). My last measure of ROM was 110 but that was two weeks ago. I have been discharged from PT but still want to get to at least 120. I am very interested in what you have to say about stretching. I have been trying to gain improvement by riding my Peloton bike and trying to lower the seat every so often to get more bend. I am spending less time stretching but I will do heel slides from time-to-time. I see by reading your posts and comments that I am not going about this the right way.
Reply
1/22/2022 01:09:41 pm
Yes, stretching is dose dependent, particularly at this relatively late stage in recovery. Typically patients have great difficulty regaining more motion beyond post-op week 6-8. If this is still your desire, I do not think the bike is the way to do it. Prolonged stretching would be 30 minutes at a time, a couple times per day, ideally. And when I say 30 minutes, this is a single, long duration stretch, not a series of multi-second bounces, as is often recommended. It will seem like a very long time because it is. I recommend distracting yourself with a TV show or podcast to help this time pass. I don't think the pool will be particularly helpful with regard to stretching either. Even doing stretches like this, at 15 weeks, the outcome is uncertain. It is worth a try, however, and (other than the time spent) there is really no downside to making the effort.
Reply
Trish
1/22/2022 02:02:01 pm
I'm coming up on 6 months post op. Still have some swelling when I overdo it a bit, to be expected, I know everyone is different.
Reply
1/22/2022 02:36:28 pm
It sounds like you may have synovitis, or irritation of the joint lining (the synovial tissue. Sometimes, when this happens, the tissues will create audible crunching sounds through a range of motion. When this is also painful, it makes sense to consider surgery. In the absence of pain, the indication for surgery is less clear. However, if you are not happy with this situation, your surgeon could consider arthroscopic debridement/partial synovectomy. This should solve the problem.
Reply
2/6/2022 12:07:42 am
Just saying thank you for sharing your knowledge. I’ve recommended your site to others.
Reply
2/26/2022 03:14:40 pm
Different patients have different pain thresholds, experience different degrees of inflammation, and have different coping skills. In spite of many comments on this website, many people do not have a horrendous recovery period.
Reply
2/6/2022 03:58:27 pm
I am 41/2 months post op from a total knee. I have full
Reply
2/26/2022 03:11:12 pm
I would expect ongoing improvement for up to an entire year, or more following surgery. It is not uncommon for the second knee replacement to seem more challenging and slower to recover than the first.
Reply
2/9/2022 08:09:56 pm
Hello, I had bilateral TKR's 11 months ago, I did 8 months of PT was able to get get ROM and strong, however, i was feeling pressure under both knee caps at the end when I was released. The problem I'm having is the pressure is getting worse. It's not pain, just pressure.
Reply
2/26/2022 03:08:15 pm
Most of the time an infection will not present as you describe. Many times pressure under the kneecaps results from inadequate rehabilitation. Check out my article on anterior knee pain. Weakness about the hips is quite common, particularly after surgery. Strengthening will usually solve this problem for you. That all being said, if you have concerns about possible infection, you should get an appointment with your surgeon for re-evaluation, and further laboratory investigation. Fevers, chills, redness about your knee, severe swelling, or wound breakdown needs to be evaluated emergently.
Reply
Dylan Shirk
3/31/2022 08:52:26 am
I’m 4 weeks post-op from total knee replacement and my ROM is between 110-115 degrees while my leg bend is about 2cm from being totally straight. There is still quite a bit of swelling compared to my non-surgical leg. I’m doing all my recommended exercises and stretching but my knee still tightens up after I rest. Will this eventually resolve or should I consult my surgeon. My therapist says the tightness is normal but I was looking for another opinion.
Reply
4/9/2022 04:32:08 pm
Tightness is normal, and expected, at this stage following knee replacement surgery. This will eventually resolve as your range of motion improves, and as you get farther along from surgery. Regaining full extension is crucial for a good result, however. Check out my knee extension exercise article to learn the prone hang technique. Best of luck to you!
Reply
Darlene
5/6/2022 11:51:43 am
Thank you for your advice. It did the trick. Left medial PKR in February 2020 - no issues. Right medial PKR on March 23, 2022. My extension was 0 immediately post-op and good strength but I have had to fight so much harder for my bend. Partly because post-op, my quad was extremely tight and hindered my bend along with the swelling. Quad muscle settled down after babying it but I could still barely push/gently force my bend (very uncomfortably) to 95- 100 degrees at nearly 5 weeks post-op and then it tightened up and I was regularly back to square one when I did my wall heel slides a few hours later. My PT was puzzled. I stumbled onto your website and started holding my stretches as you described --for prolonged periods -- and noticed a big difference within days. Passive ROM is much better and I can fairly easily actively bend to 122+ degrees with my wall heel slides and I expect my ROM to continue improve before my 6 week post-op next week. What a relief - so thanks! I almost wonder if having a strong quad pre-op contributed to my quad strain (Makoplasty with incisions in the quad and shin.) With my left medial PKR I limped for 6 months so my quad had atrophied so maybe that is why my bend came more easily? However, all in all this recovery seems better having strong muscles pre-op. I appreciate your insights.
Reply
Danny Nelson
5/29/2022 01:52:35 pm
I had total knee replacement on my left leg 4 years ago. I got good leg extension and bending in the beginning. Then I went back to work. 12 hour shifts on concrete. I progressively began to lose the ability to bend my knee. It became hot and swollen. Went back to surgeon over and over. He finally after 2 years did blood test, Drew off fluid for testing and a bone scan. All came back normal. So he put me to sleep and manually forced it to bend. All good til I went back to work. Same issues, swelling, hit and loss of ability to bend it. Went back to surgeon 6 months later and he tells me he feels it's scar tissue & under the conditions I work, it's not going to get better. So I've lived with this til 2 months ago. I took early retirement because of my knee. I go back to surgeon. He again performs blood tests, bone scan & has fluid drawn off to test. All come back ok except bone scan. He says it's a bit off and doesn't tell him exactly what's wrong. So he again puts me to sleep and manually forces it to bend. This time putting me on strong steroids. Now I don't want it to stop bending again and I certainly don't want the pain, swelling and heat!! What can I do now? I'm taking PT and I am doing the exercises they recommend every waking hour. Please help me!
Reply
7/9/2022 02:45:19 pm
If you have truly put forth proper rehabilitation effort after each of these interventions and then progressively lose motion, I would make sure you have ruled out material sensitivity. Perhaps get referral to an allergist. Check for all materials used in your knee replacement. Typical prostheses may include: titanium, zirconium, nickel, cobalt, chrome, polyethylene, polymethylmethacrylate.
Reply
Dan Greitzer
6/1/2022 12:13:17 pm
TKR R-Knee 2/22/2022
Reply
7/9/2022 02:38:22 pm
The best stretch to regain extension is prone hang. CPM is not typically able to get you to full extension, it is fine for mid-range motion however.
Reply
Mary C Long
6/6/2022 10:34:08 am
I had a total knee replacement on May 2nd, 2022. I am exactly five weeks since surgery. The bend in my knee is only at 55. I go to physical therapy 3 times a week and I do an exercise routine to aid the bending, three times each day. I feel as if there is a vice or a tight band around my knee and my leg feels like it is filled with bricks. I am taking Gabapentin, Celebrex, Tramadol and extra strength Tylenol. Is it possible that the knee replacement is too large or am I just delayed? If I don't show Improvement, around the eighth or ninth week, they will have to do a manipulation. I am working I'm getting the bend because I don't want to have the manipulation. Naturally, if I have no choice, I will do it. Prior to surgery I was an active person, weighing 106 lb so I am not lugging around any extra weight. Thank you.
Reply
7/9/2022 02:35:40 pm
It is extremely unlikely your knee replacement is the "wrong size." However a modern replacement is done (manually, navigated, robotic) every bone resection is carefully measured. This question arises occasionally- but is almost never the issue with stiffness after surgery. At the end of a properly performed total knee replacement knee range of motion is unrestricted (0-140) with very few exceptions. A surgeon would need to work very hard to perform a knee replacement that only flexes to 55 degrees. Technically, it would be nearly impossible to insert/assemble the tibial implant with this degree of stiffness. Insertion of the tibial component requires at least 90 degrees of motion. So, no, I do not think most cases of stiffness following knee replacement surgery are due to a surgeon choosing the "wrong size" implant. The problem is with rehabilitation. Some people struggle. This is precisely why I started this website. It does not feel natural to patients to stretch early after knee replacement, and yet it is essential.
Reply
6/8/2022 09:18:03 am
It's good to read an article that so clearly has been written by an intelligent person. You are a very good writer. This is great.
Reply
Scott Robinson
6/10/2022 05:00:31 pm
I am a 63 yo male, former runner, 5'4" in good shape s/p RTKR in 2014 that ultimately resulted in severe scarring of the quad tendon. The initial replacement included metal hardware placed behind the patella with the polyurethane attached behind the metal. Unbeknownst to me at the time the metal hardware was placed asymmetrical over the patella and tilted. It was a stiff knee from the start, but I could still live my active life. In 2019 I had a couple cysts on the lateral aspect of the knee removed that had occurred at separate times. The knee worsened, but it still took about 9 months before someone opened up the knee and found that the polyurethane had split in two, and those two pieces were floating freely in the joint. There was also severe, diffuse metallosis of the joint capsule from the patellar metal scraping the femur.
Reply
7/9/2022 02:08:35 pm
You have had a very unusual/difficult time with your knee replacement. A thickened quadricep tendon with a posterior stablized total knee can sometimes catch within the intracondylar notch when extending the knee under load from deep flexion into extension. This is called patellar clunk. If you simply have a thickened/degenerative quad tendon (severe tendinosis), this could cause pain, and could be improved with open debridement/repair. Of course this would then require significant rehabilitation. We must be cautious, however, as your knee has already experienced multiple surgeries plus the metallosis. If the problem is simply stiff, non-complaint quad tendon, and not stiffness due to scarring in the suprapatellar pouch, your knee is probably best left alone. In my opinion, you need to be carefully examined in the office, and your most recent imaging studies evaluated. I know of no orthopedic surgeon that specializes in scarred quad tendons, but I would expect any arthroplasty specialist should be able to help you.
Reply
Michelle Tate
6/15/2022 02:19:10 pm
I had total knee replacement 6 weeks ago. I have stiffness and my doctor wants to do a manual manipulation. With the help of the dynasplint I have gotten my flexion up to 115. When the stiffness kicks in, it feel like I can do nothing. How do I prevent stiffness? When will it go away so I can make more progress? Does MUA prevent stiffness?
Reply
6/29/2022 12:48:59 pm
Stretching consistently is the only way to prevent stiffness. At this point the manipulation will help you "catch up" in regaining range of motion. It is a treatment for stiffness, as opposed to preventing it. You will need to continue stretching after the procedure.
Reply
6/15/2022 06:54:03 pm
I like the tip that you gave that the knee has tissue planes as it is a complex joint. My sister told me a couple of days ago that she was having difficulties with her knee pain because of arthritis, and she asked if I had any idea what would be the best treatment option. Thanks for this helpful article, I'll tell her that consulting a trusted osteoarthritis treatment service can help provide more information about the treatment process.
Reply
Fatima
7/8/2022 09:04:19 am
Hi, my dad had a total knee replacement 5 weeks ago. He is doing exercises during the day and is able to claim stairs up and down and walk reasonably well with crutches. However, he can't stay too long in the same position, siting or laying down. For example, he needs to get up sometimes during mealtimes because his knee starts to feel uncomfortable and during the night he keeps waking up because needs to change position in order to sleep again. Is this normal at this stage and are there any exercises that could help improving this situation? Many thanks in advance
Reply
7/8/2022 07:37:48 pm
Difficulty sleeping, and the need to keep moving is quite common following major surgery. Ice, and anti-inflammatory medications can be helpful. Most importantly, this will improve with time.
Reply
Dolly Sharma
7/28/2022 05:34:20 am
Hello doctor, I had distal femoral medial closing wedge osteotomy to get my right knee straightened. I had knock knee in my right leg. I did not have arthritis, no pain, no gait issues prior to operation. I just did it for cosmetic purpose and future health of my knee. I am 26 years old. It’s been 4 months since my operation and I am at 110 degrees of flexion. My extension is fine. My doctor said with continued exercises my flexion would still improve as flexion is a gravity based movement but I have read mostly that after 3 months it’s rare for the joint to flex more. But my surgeon says otherwise. He says it will improve if I continue my exercises, which I am doing. Also my doctor mentioned that to achieve terminal flexion we can take out the plate after one year. Please advice.
Reply
7/29/2022 07:48:39 am
I agree with your surgeon.Your surgery was quite different from a total knee replacement, as your joint was not opened/reconstructed. If you keep working on stretching exercises, you may regain motion for up to an entire year from surgery. I would not expect the plate to block any motion, and would not plan on removing it, unless there was an obvious problem with it.
Reply
Dolly Sharma
8/2/2022 05:48:34 am
Thankyou doctor for your reply.
Nancy Lamb
8/14/2022 09:31:33 pm
I sure wish I'd seen this before my surgery, or shortly after. I did not realize I should hold the extension stretch for so long...and was told 3 x a day for pt RX..
Reply
Alicia Anderson
8/23/2022 11:32:19 am
Dr. Gorczynski,
Reply
8/24/2022 12:14:37 pm
JAS brace may be very helpful for the flexion contracture (lack of extension) you have. Assuming your surgeon feels you are adequately healed from the fractures, then a manipulation could be considered, with or without a steroid injection. If you are still on crutches due to inadequate range of motion, regaining motion needs to be the major focus. If you can not bear weight due to ongoing pain, perhaps repeating the MRI scan to ensure there is not additional intro-articular injury (for example a displaced bucket-handle meniscal tear) blocking your motion. The severity of the stiffness you are experiencing is unusual at this stage following an injury like you describe.
Reply
8/24/2022 08:05:15 am
What a great Thank you for the article you've written. This is useful and well-thought out information with thought-provoking viewpoints and content.
Reply
Hello Doctor
Reply
9/6/2022 03:54:29 pm
It sounds like this could be happening due to quadricep muscle weakness. After 2 months in a brace, and then working hard to regain range of motion, I would expect your muscles to be very much weaker than normal. I would expect you to make progress for many months as your strength improves.
Reply
Patricia Mayfield
9/24/2022 07:06:05 am
Dr Gorczynski, I had both knees total replacements done one in May 2022 then one in July 2022. Theraphy was going great and I was for the most part pain free. Then on September 9th I came down with Covid and missed two weeks of theraphy. Both knees ache especially when bending and straightening but I still have good range of motion.
Reply
9/24/2022 05:12:48 pm
COVID can cause severe inflammation within your body. I have seen many patients with joint pains that they associate with having had COVID, and also with the vaccine. This is observational data only, I am not currently aware of any published study documenting or explaining this. But you are not alone. Consider using ice/anti-inflammatory medication if you can tolerate it, and do your best to maintain range of motion until you see your surgeon.
Reply
Nick Bannister
9/28/2022 11:21:15 am
Hi Dr
Reply
10/23/2022 11:03:56 pm
I would not expect you to require a manipulation if you are able to achieve 120 degrees of flexion passively. Even if it is painful. The key is to make sure you maintain this range of motion while your knee continues to heal. Once fully healed, your pain would resolve and your motion should be maintained.
Reply
Tianna
10/16/2022 07:17:06 pm
I tore my acl in April of 2021 waited until April of 2022 to get ir repaired, after 5 months had scar tissue removal done in September. I am now 4 weeks post opp and it seems I am stuck at 95 degrees. Does anyone have any pointers for reaching full range of motion again?
Reply
10/23/2022 08:40:01 pm
Long duration stretching, multiple times per day, no days off. Ice after stretching. Unfortunately, there is no shortcut.
Reply
A Bhattacharya
11/4/2022 05:00:58 am
My mom got operated 73 days back for a distal femur fracture B2 type, with screws and titanium plate...her knee is bending only a bit about 10 degrees....cant bend due to pain and swelling.She can lift up her leg straight in the air ,doing knee presses, ankle rotations and trying hard, but knee is not getting bend in 90 degrees .please help
Reply
11/6/2022 03:24:40 pm
It sounds like she is very behind schedule. Unfortunately, I can not give much advice without seeing xrays. Assuming her fracture has healed, and there is no infection, I would consider using a progressive static brace like JAS. It is best to discuss the situation with her surgeon.
Reply
11/17/2022 07:54:32 pm
That makes sense that there is a lot of inflammation involved with knee injuries. My cousin has a bad knee injury. He might need surgery.
Reply
Angie M
12/1/2022 10:57:16 am
Hello Dr Gorczynski,
Reply
12/4/2022 05:02:43 pm
At only 3 weeks postop, it is highly unlikely that you have already developed arthrofibrosis. This is dense scar tissue that completely invests your knee joint. There has simply not been enough time for this to develop. I have no experience using a laser to help with range of motion. Unfortunately, my recommendation is to stretch more frequently, for longer periods, and make sure you relax your quadriceps muscles while stretching. There is no shortcut to a good result. Stretch, stretch, stretch. Ice and anti-inflammatory meds (if you can tolerate them) may help, but stretching is the key. The reference to teeth gritting suggests anxiety, muscle tension is holding you back. I recommend you try your best to avoid these issues.
Reply
Debbi
12/13/2022 09:34:43 pm
Hello DR.Gorczynski,
Reply
12/16/2022 08:28:39 pm
0-105 is just fine range of motion for a 2 week old total knee replacement. Perhaps your 5 seconds stretching is just fine for you. Some patients have an easy time and stretching for only a few seconds works for them. In my experience, most patients need much more time at the endpoint to progress nicely. Doing 51 exercises (17x3) each for 5 seconds means you are spending a total of 4 minutes and 15 seconds stretching cumulatively each day. That does not seem adequate to me. I am not sure what all of those 17 exercises are, but I am willing to bet they are not all working on knee range of motion. This is because the knee needs to do 2 things after knee replacement surgery. Flex and extend. So my recommendation would be to focus on flexion and extension. You describe full extension. This is great. Simply maintain what you have by pushing your knee fully straight a few times each day. As long as you maintain full extension like that, there is no need to spend any more time on extension. You want more knee flexion. This will only come by stretching deeper into flexion. Stretching is dose dependent. This means the more you stretch, the better the result. So, this is why I recommend long duration stretching. I want my patients to get excellent results. It is not possible to over stretch. I have had patients regain completely full range of motion in their replaced knee by diligent stretching. They were able to touch their heel to their buttocks. These are clearly outliers, but I use them as an example here to suggest stretching for longer durations is not only safe, but generally much more effective for post-op total knee patients regaining excellent range of motion. A stretch that is not uncomfortable is not really a stretch. Push the stretch until is is unpleasant. Relax into the stretch, and long for as long as you can tolerate it. Over and over throughout the day, every day. That is all that is needed. I bet most of those other exercises are meant for your hips, ankles, gait, etc. Certainly do those things, it will only take you a couple of minutes each day. I recommend stretching for a total of 60 minutes, minimum, each day for the first 6 weeks to get a good result.
Reply
Debbi
2/5/2023 06:57:57 pm
Thank you so much for your detailed reply! You are correct, out of the 17 exercises, extension was only: prone, seated and standing quad squeeze/press; and flexion was only prone heel slide and seated heel slide. At my two week I asked my doctor what he thought, and he said why not do both long duration slow stretches and keep doing the others, so I did. I went way past the pain for the short ones and mild discomfort for the long ones. Now at 9 weeks, I got to less than zero extension and 137 flexion. I was able yesterday to hike a mountain for 70 minutes with no discomfort. I have two questions. At 4 weeks when doing prone quad curls with the strap, for the first few times, rather than feeling a stretch, it felt like my skin was ripping open. After that it felt like stretching. Was this scar tissue breaking? 2/16/2023 10:12:23 pm
This indeed may have been some scar tissue tearing. Your range of motion is outstanding at this point! If you do not bring your knee through a full range of motion frequently, then you might lose some range of motion. This does not mean you need to dedicate lots of time to stretching, just that you should maintain what you have with a few minutes of stretching each day for the next couple of months. I would recommend doubles tennis over singles for the best long-term durability of your new knee replacement.
Mike Kogan
12/15/2022 08:49:21 pm
Doc I love your videos and interaction with tkr patients. I just had tkr and have had 2 prior knee surgeries that led to my bone in bone status (meniscus then ACL recon at age 35). The knee is so much harder than a shoulder tenodesis or ecrb repair to rehab imo. I'm 60 years young, 6'4" and your videos and advice have really helped. At 3 weeks I have great extension and 110 flexion and am following your advice rigorously. Most Ortho surgeons do not have your focus on rehab and leave it to the PT folks. My question is what can I do to get rid of the swelling more better faster. I do RICE excessively and own a game ready machine. Once again thanks so much, more Ortho surgeons should be like you!
Reply
12/16/2022 08:44:30 pm
Thanks for the positive feedback! I think you are doing great for 3 weeks postop. And, I agree, knee rehab is harder than shoulder rehab for sure, though some would argue that rotator cuff rehab is a close second. The real problem with knee rehab is the relative hard endpoint around 6 weeks for range of motion recovery. This adds an element of stress/anxiety that is fairly unique to knee replacement. It sounds like you are already doing the proper things: ice, elevation, compression, and stretching properly. Younger patients, particularly men, seem to have a more aggressive inflammatory response. This means more heat, swelling, and stiffness. The only other thing that will definitely help you out, is time. Your body goes through an aggressive inflammatory cascade following surgery, it will gradually resolve over the next few months. While anti-inflammatory medications may temporarily suppress this response a bit, your body will naturally settle down with time. Best of luck with your continued rehab. I think you are right on track for a great result!
Reply
Dave Warren
12/31/2022 09:07:54 am
I'm 9 months post TKA, and having difficulty with my distal quads, their always tight and knotted, I continue to do PT 3 days a week on my knee, hamstring extensions, quad extensions, seated leg press, aductors, abductors, air squats, calf raises, w/o weight, stretching of hamstrings and quads, massage therapist, deep tissue, went to an acupuncturist, she put electrodes to the needles, tens unit, still have lots of discomfort. with the quads, when I sit ride, sleep, my knee fees normal, but when I walk it feels like I have an Ace bandage extremely tight around my knee. My surgeon shrugs his shoulders says well it will take 18 months or so to get to normal, I'm not a normal guy, I've researched can't find any information on this issue I'm having, Can you help?
Reply
1/16/2023 11:57:11 am
It sounds like you are doing well for this stage. I would expect continued improvement for at least a year following total knee replacement surgery. A recent article followed patients who were not satisfied with the outcome of their knee replacement at one year, and they found increasing satisfaction for up to 5 years post-operatively. So, keep exercising, and expect continued improvement in how it feels on an ongoing basis.
Reply
Donna Francois
1/5/2023 08:52:27 pm
9 months post right knee replacement. I am unable to go up and down stairs normally.It’s feels uncomfortable when I try to go do so. Knee does not sturdy enough yet . Is this normal? What can I do to improve this.
Reply
1/16/2023 11:41:02 am
This is absolutely not normal. There are a variety of issues that can occur with total knee replacement, and rehabilitation that can interfere with good functioning. Unfortunately, I am unable to give you an exact diagnosis and plan with the information you have provided. I recommend you follow up with your surgeon for X-rays, and examination. And if no recommendations are made, I would recommend getting a second opinion because what you describe is absolutely not what I would expect at 9 months following total knee replacement.
Reply
1/24/2023 10:51:17 pm
This is really an beneficial article, thank you so much for the post.
Reply
Beam Doen
3/17/2023 06:42:13 pm
I am a 57 yo male who had a complete quad tendon rupture repair on my left leg (transosseous). I have been following the MA General PT rehab protocol (2 weeks in full extension, weight bearing as comfortable, heel slides; 2-6 weeks active and passive flexion and strength building, tissue massage 2xdaily etc. I am at 54 degrees flexion ROM coming into my 7th week (started at 30). I have been diligent about PT but seem stuck and am concerned that slow progress is a problem. I read above that I should be concentrating at the end of the ranges. I will start doing that. But should I be concerned with the slow progress and my current ROM? Is a MUA a likely outcome? If I'm pushing myself to the point of pain tolerance, is that fine or might that not result in progress? What else shold I be thinking about?
Reply
3/23/2023 04:14:31 pm
I would prefer you to be at 90 degrees of flexion by 6 weeks postop from the quad tendon repair. Compared to total knee replacement, my experience suggests that range of motion will continue to return for a longer time period after this surgery. Nevertheless, I would encourage longer duration stretching while trying to relax the quadriceps as much as possible. I have never had to perform manipulation under anesthesia on a quad tendon repair. While I am sure this has been done by someone, sometime, it is certainly not a frequent need. When your motion is not progressing, you need to increase your "dose" of stretching (most effectively) by increasing the duration and/or frequency of stretching.
Reply
Beam Doen
3/31/2023 08:10:24 pm
Thank you. That is very helpful. I try to stretch all day at work by putting pressure on my knee by pressing forward from the chair or trying to pull it toward me. Then when i stand up I have to shake off the ache before i feel comfortable taking a step. I also found when driving I can keep moving my seat up inch by inch holding it as long as I can until I cant take it on my left leg. Sometimes my trips are an hour or longer. I am also now doing quad sets and hamstring passive and active stretches. I made 3 degrees of progress last week, and 3 the week before. So now I am at 8 weeks and 60 degrees. Progress, but slow. 5/7/2023 03:26:27 pm
As long as you are making some progress each week, you may ultimately regain full range of motion. You are still very stiff, unfortunately, so it looks like progress is very slow. As opposed to knee replacement surgery, patients who have had quadricep or patellar tendon repair often are able to regain motion for much longer than the typical 6-8 week period after knee replacement. I am concerned that you will not regain full range of motion based on where you are now, and how difficult the process has been, but I hope you prove me wrong. I firmly believe that the more cumulative time you spend stretching, the better your individual outcome will be.
Reply
Betty P.
4/24/2023 08:59:26 pm
Hi there! Finding this website very interesting.
Reply
5/7/2023 03:06:01 pm
I don't understand why your postop knee range of motion was limited to 105 degrees. If this is indeed the case, then that is truly the maximum you can expect to obtain no matter how you stretch. That being said, 105 degrees should be adequate for most functional activities. It sounds like you had a severely valgus knee (knock-kneed) before surgery. It sounds like fairly standard releases were required to correct this. FYI, ACL is generally completely removed in the vast majority of knee replacements, so this particular portion of your operation was standard. I would recommend continuing long duration stretching as much as possible, though beyond 6-8 weeks any gains are likely to be small. Best wishes, and feel free to give us an update a few months down the road if you wish. Regardless of your ultimate range of motion, your knee should calm down month by month, and feel better and better for up to an entire year from surgery, or more.
Reply
Betty P.
5/7/2023 03:47:54 pm
"severely valgus knee (knock-kneed) before surgery"
Sabin
5/3/2023 02:31:46 pm
Thanks doc. Your technique of holding the stretch for minutes really worked for me. I am 5 weeks post op from ACL reconstruction and i was at 102 degrees flexion. I gained 14 degrees in just 2 days. Now im at 116 flexion. Extension is also getting easier and i can get to zero fast. Before i was struggling at around 4 degrees extension without PT manipulation. My surgeon was saying i was progressing slow before and said manipulation is a possibility if i dont improve. Now i think i can easily add 10 more degress to reach 125 before the 6 week end. I will push for more and go for 130-135 if I can. I will update in one week. I wish more PTs taught this. My PT focused on high reps (30) and short stretch (5-10s) and i always felt stiff and lost progress. Now, my pt says my knee feels much better. Not stiff anymore and knee moving fluidly.
Reply
Sabin
5/10/2023 10:15:58 pm
Back after a week. 6 wks post op from ACL reconstruction. Been doing long stretches as you suggested. Was at 116 degrees at end of week 5. Now at 128 and extension is getting easier. Thanks doc. I know this post is mostly focused on knee replacement but wanted to share it worked for me too. Just a quick question, whats the max flexion i can expect and around what time frame? Thanks. I am 30 yrs male. My good knee can bend upto 155 degrees.
Reply
6/20/2023 07:39:04 pm
So happy to hear you are making good progress using long duration stretching! Keep up the good work, and enjoy your new ACL!
Ricardo
5/8/2023 05:04:16 pm
I have underwent an MPFL ligament reconstruction. 3 weeks i have gone 100° but does the pain stop at some point because everyday bending my knee to flex the ligament is so painful. And as well i am aiming for 130° full mobility as i am an athlete. I use warm water to stretch my muscles to cope up but nothing to stop the unberable pain , as the doctors also have rmtold me to bare the pain during bending.
Reply
6/20/2023 07:37:37 pm
The pain is expected to get better with time. Consider 12 weeks as a milestone where inflammation generally is much reduced. Bearing with the pain while stretching is very important, but holding stretches for longer periods of time with less force may also be better tolerated, and thus more effective.
Reply
Vera
6/3/2023 05:05:21 pm
Hello Dr!
Reply
6/20/2023 07:43:43 pm
You don't mention how much flexion you have. Assuming it is functional (>110), and all you really need is more extension, consider using a static splint like JAS. I find these to be more effective in regaining terminal extension. If your flexion is also suboptimal, then perhaps revision surgery might be needed. This is not an easy, guaranteed way to go. There are significant risks including infection and more stiffness. If you ultimately decide to go that way, make sure you rehabilitate much differently afterward, using long duration stretching immediately.
Reply
Anika Singal
6/8/2023 02:43:24 am
I am 39 year old female and had patella fracture 11 weeks back. The recovery is very painful and my incision still has still burns.
Reply
6/20/2023 07:46:26 pm
The hardware used to repair patellar fractures is commonly prominent and irritating. Once you are well healed, and well rehabilitated, this hardware could be removed. This can be done 6 months to a year following surgery at the earliest.
Reply
Hello,
Reply
6/20/2023 08:00:00 pm
While it is certainly possible that cement fragments are irritating your knee, unless there is a ton of cement left behind, I doubt a few pieces of cement are causing you so much difficulty. How is your range of motion? Have you had an ultrasound to rule out a Baker's cyst?
Reply
Belle
6/30/2023 01:06:16 pm
Hi I sustained a minimally displaced patella fracture nearly 7 weeks ago due to a strong contraction in my thigh muscle. No damage to tendons as was able to do a straight leg lift unaided. I have been in an ROM hinged brace 24/7 since diagnosis. It is currently set to 70 degrees however I am probably only managing 50 degrees at a push. My knee is still quite swollen, tight and stiff - I have been told to continue wearing the brace for another 6 weeks(!!!) with the aim to have ROM beyond 90 degrees at that stage. I start physio in a couple of days (in the UK so NHS) but the only advice I have had so far is to keep bending the knee up to the limitation of the brace. No real technique, just sit on the edge of the bed and try to bend the knee by sliding my foot on the floor towards me. And do this every hour for a minute? My knee feels like it will pop out if I really push it and some discomfort in various places on the knee - is this normal due to tightness/swelling? Pain is not too bad now but I am just concerned that I will open up the fracture which is healing by pulling it apart if I really try to push the ROM? Will I ever get to full ROM again? I was not given crutches so I am kind of limping but trying to walk as normally as possible (weight bearing from the start). I just can’t see the light at the end of the tunnel here! Any advice would be appreciated, thank you.
Reply
7/2/2023 07:30:12 pm
At 7 weeks from the injury, the fracture should be healed. I usually demonstrate radiographic healing around 6 weeks or so from the injury. Once there is bony healing seen on x-ray, you should be able to advance range of motion progressively without limitation. If you are only starting with 50 degrees of motion at 7 weeks from the injury, stiffness and pain is anticipated. You should be able to regain range of motion for significantly longer than we typically see after knee replacement surgery. You may never regain totally normal range of motion after such an injury, but you should be able to regain functional range of motion.
Reply
Raamael
7/30/2023 07:13:17 pm
Hello,
Reply
11/4/2023 11:32:46 pm
What you describe is totally normal for 6.5 weeks postoperatively. Simply keep stretching as described throughout this website, and on my videos. This, plus time should get your knees feeling good. Expect the feeling of stiffness to gradually settle down month by month for an entire year. Many people feel a major shift around 3 months postop. By this point the inflammatory process that gets fired up after surgery has mostly resolved.
Reply
Nicola Robertson
8/18/2023 02:31:32 pm
Hi there,
Reply
11/4/2023 11:29:24 pm
I suggest you browse this website, including the video section. All knee range of motion exercises I suggest for knee replacement rehabilitation should be helpful to you. Focus on long duration endpoint stretching. I describe this thoroughly in these videos. I think this will be much more helpful than trying to describe it to you in a comment.
Reply
Amy
8/19/2023 08:05:02 am
My original injury was a displaced patella fracture (3 pieces) that was fixed with screws almost 9 months ago. I was able to get almost full range of motion back afterward, but the screws were sticking way out so I just got those removed. I am about two weeks out after the screw removal surgery, and I am not supposed to bend past 90° for the first six weeks. There is a lot more swelling and fluid and stiffness that I anticipated with this second surgery. Is it likely I’ll be able to get my full ROM back after the six weeks?
Reply
11/4/2023 11:26:47 pm
Yes, I would expect your range of motion to come back to where you were prior to the removal of hardware surgery, in spite of the restricted range of motion recommended for the initial 6 weeks post. Stiffness is much more likely with intra-articular surgery (knee replacement) as opposed to superficial surgery (removal of patellar hardware). This does not suggest your surgery is not painful, simply that the joint itself was not traumatized significantly. It is for this reason that I would not expect stiffness to be much of an issue in your case.
Reply
Catherine
9/7/2023 07:21:54 pm
Hello, Thank you very much for this forum. My situation: Right TKA 3 months and 1 week ago...fell that night and pushed knee replacement to the far right, detached the quad and broke my fibula at the ankle. Had another surgery the next day, wore a leg brace and a boot for several weeks.
Reply
11/4/2023 05:35:46 pm
What a difficult time you've had. It is impossible for me to say exactly what is going on since I can not examine you. Usually posterior knee pain is due to tight posterior capsule/scar tissue that has formed in the back of the knee. Generally, stretching through it, and time/healing will solve this problem. Posterior thigh pain (if it is around or just down from the bone you sit on) is likely hamstring irritation/tendinosis. If your hamstring is indeed tight down by your knee, it makes sense that the other end could be tight as well. Stretching your hamstrings should solve both problems. I would definitely not stop stretching your knee, however.
Reply
Gayle Luebke
2/14/2024 09:46:22 am
I am 54 years old and 11 weeks out from total knee replacement. I am starting to feel better but when I lay on my back and try to bend my knee it feels like it locks up and pain radiates from the outside of the knee and down my shin when I hit around 118-122 degrees. Is that the end of my range or is something else going on? One other thing that is happening is that my hamstring is so tight, from the amount of straitening they had to do with my leg, that it feels like it catches and releases like a rubber band. They said that will get better over time. Not sure if that has anything to do with the pain when bending?
Reply
3/17/2024 07:21:06 pm
This sounds like a normal part of the rehabilitation process. I agree that it should improve with time.
Reply
Debbi Dixon
2/15/2024 11:56:31 am
I’m 1 yr 3 months post TKR, my range of motion is fine about 140 and I have no pain or discomfort at all in my knee at all. I play tennis like four times a week but still I cannot be on all four with my knee, when I touch my knee to the ground it feels like I’m setting it down almost on sharp gravel or something. Even on memory foam. the only thing that I can possibly do is, I have a 5 inch beaded pillow where there are always beads between my knee and the floor. The only thing I can think is now there’s not enough tissue between my kneecap and the skin? doesn’t feel that much harder than the other knee, though :-(
Reply
3/17/2024 07:19:43 pm
It sounds like you may have a neuroma in the front of your knee. This may gradually improve over time. Alternatively, your surgeon could inject this area with some cortisone to reduce sensitivity. Worst case scenario, the hypersensitive nerve end could be resected.
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
Dr. GorczynskiOrthopedic Surgeon focused on the entire patient, not just a single joint. Categories
All
|

 RSS Feed
RSS Feed